Wellen’s Syndrome involves an ECG pattern representing a significant major coronary artery stenosis. More specifically, a Left Anterior Descending(LAD) artery stenosis. In most cases this is proximal, but it may be mid or distal LAD.
It actually represents a reperfusion of the vessel and is one more reason to perform serial and painfree ecgs. If not recognised and treated, it can result in up to 75% of patients having an anterior wall myocardial infarction within days/weeks.
How to Recognise the Pattern?
The peculiarity of this ECG pattern is that it may not appear when the patient has pain. In fact the only finding when the patient has chest pain, may be a small negative deflection at the end of V1 and V2 . The T waves become deeply inverted when the patient is pain free and represents a reperfusion of the myocardium. Cardiac enzymes will be normal in most cases or mildly elevated.
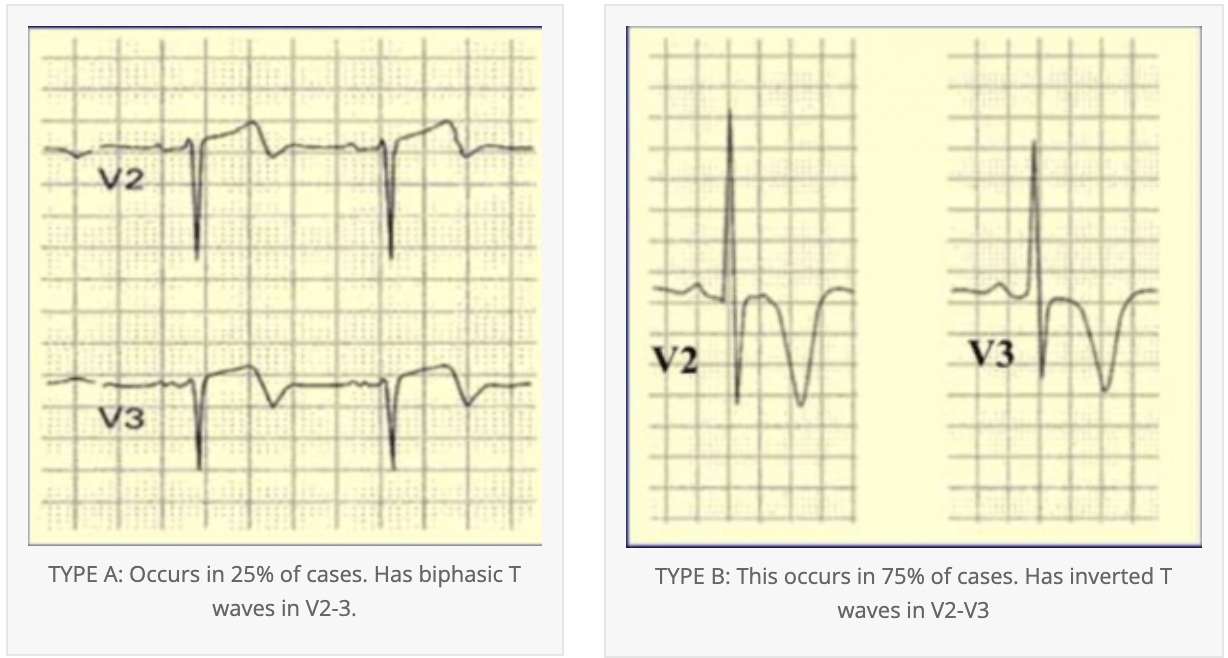
Below are the two key ecg patterns in Wellens’.
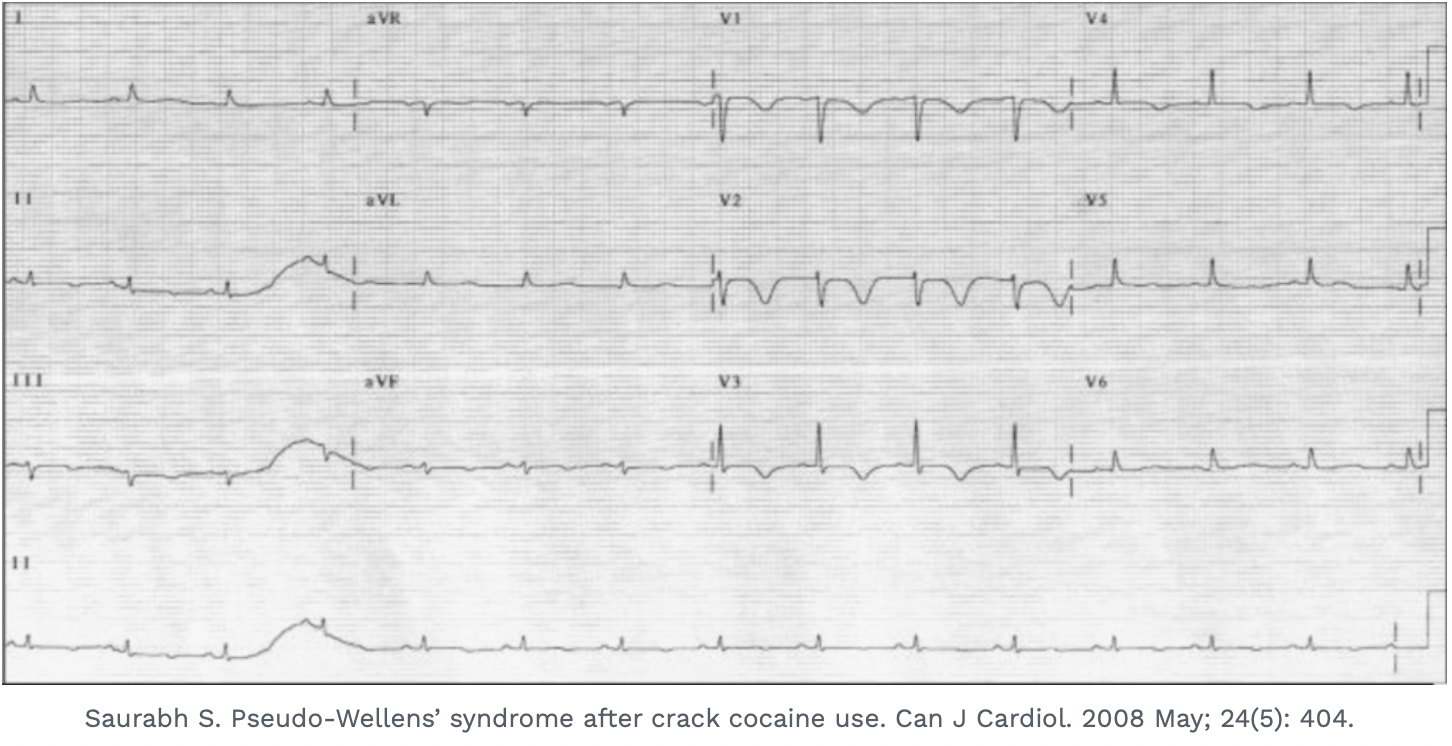
What is Pseudo-Wellens’?
So if there is LVH we cannot diagnose Wellens’ Syndrome on ECG. The patient may however still have ischaemia, so beware. One more thing that is different in Pseudo-Wellens’, is that the changes are more lateral i.e.., V3-V6, whereas in true Wellens’ they are at V2-V3.
The ECG below is a very good example of the ‘pseudo’ pattern. The biphasic waveforms are due to left ventricular hypertrophy. They are also more lateral than the true Wellens.
Other mimics also exist
Even though we may consider them as mimics, our first priority always is to rule out ischaemia first. The diagnosis of a pseudo-Wellens’ is a diagnosis of exclusion.


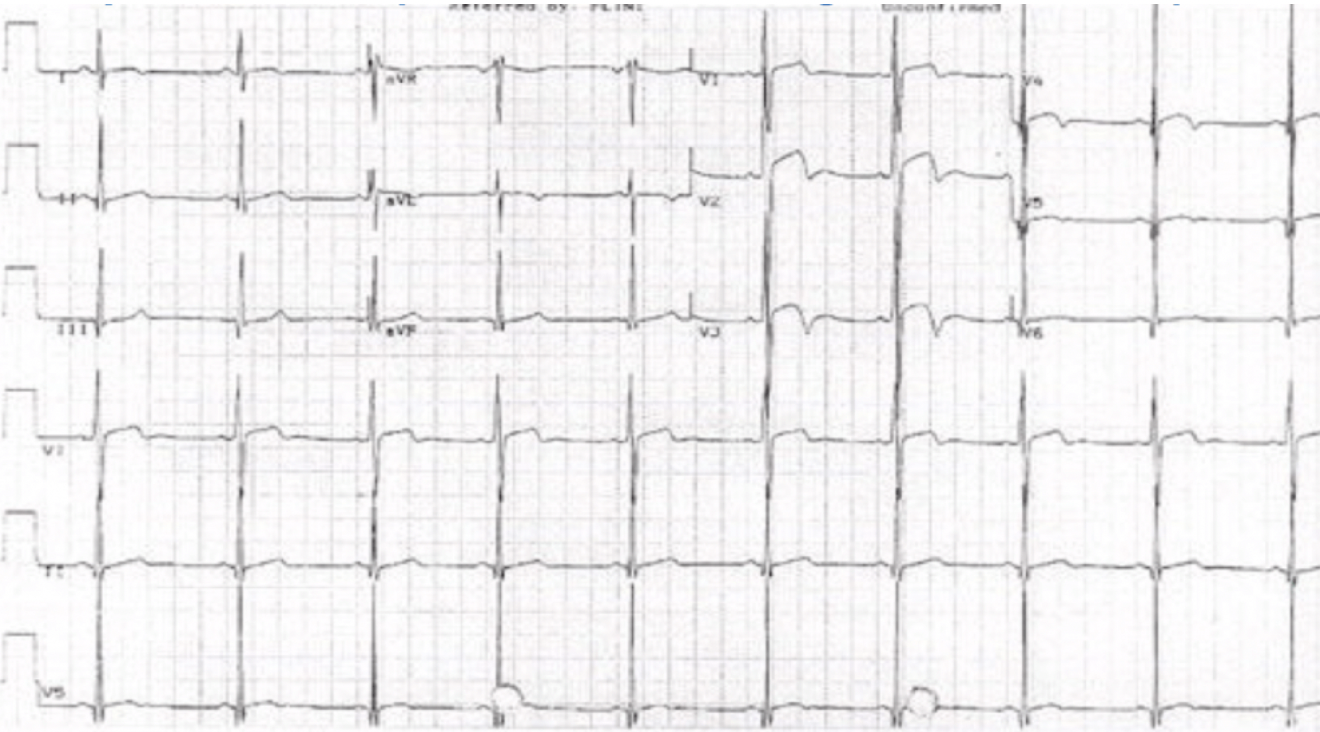
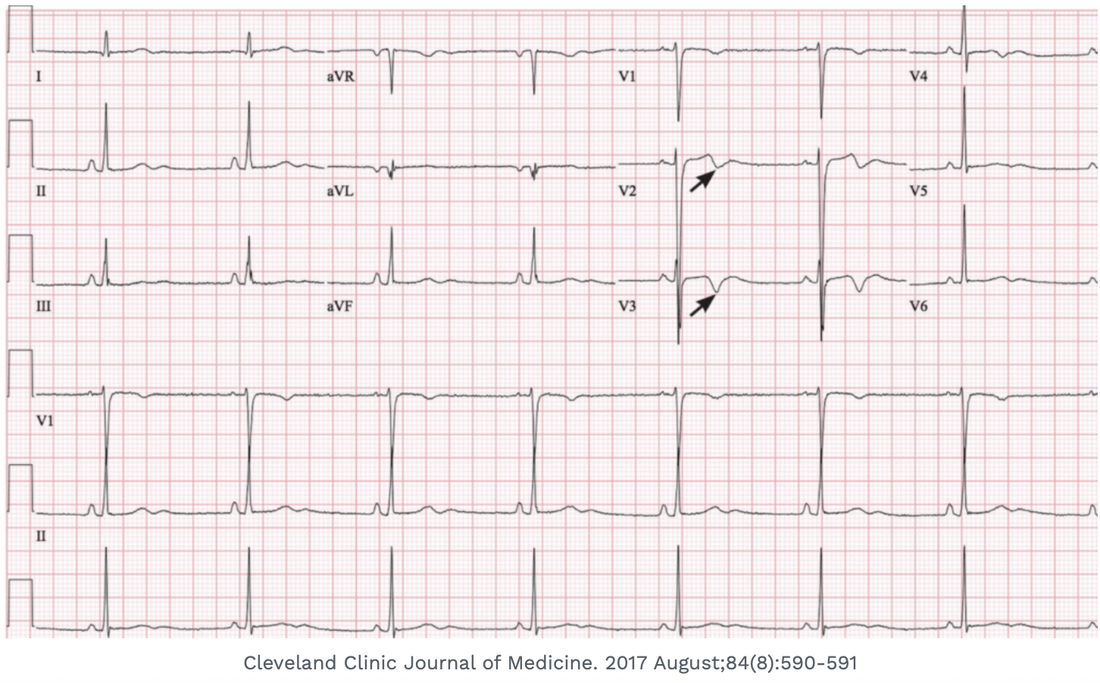









for the patient of LVH above … his ECG meets electrical criteia of LVH…V1 + V5 35 mm..