The 2022 Guidelines for the Management of Spontaneous Intracerebral Haemorrhage have just been released by the American Heart Association and the American Stroke Association.
This is a brief summary. Read the journal article here: Stroke 2022 Jul;53(7):e282-e361.
I will be covering all the management aspects associated with Intracerebral Haemorrhage at the next two EMCORE Conferences(Fiji, Queensland).
Once you’ve read the summary below, come back and watch this lecture from 2017.
Introduction
10% of strokes are due to intracerebral haemorrhages (ICH). This type of stroke has a mortality of 30-40%. It increases with age and with anticoagulation. Approximately 73% of ICH is attributable to uncontrolled hypertension.
Two cerebral small vessel pathologies that account for the majority of ICH are; arteriosclerosis and cerebral amyloid angiopathy.
How do Bleeds cause brain injury?
Brain tissue is injured by:
- Direct pressure secondary to the expanding mass lesion
- This causes local compression of surrounding brain tissue and
- Mechanical injury from raised intracranial pressure, hydrocephalus or herniation
- Secondary physiological and cellular pathways that are activated by the haematoma and the metabolised blood products include:
- Cerebral oedema
- Inflammation
- Biochemical toxicity of blood products such as haemoglobin, iron and thrombin
Diagnostic Assessment
Labs
- Complete Blood Count
- Low platelet counts of <10,000 may cause ICH
- Thrombocytopaenia is associated with higher mortality in patients taking antiplatelet agents.
- Admission anaemia is associated with haemorrhagic expansion and worst outcomes
- Low platelet counts of <10,000 may cause ICH
- Coagulation Studies Prothrombin time/ partial thromboplastin time/INR
- Troponin: Elevated troponin on admission may be associated with increased hospital mortality.
- Renal function: Renal failure on admission is associated with poor functional outcomes and in-hospital mortality.
- Glucose: Hyperglycaemia on admission is associated with both short term and long term mortality.
Imaging
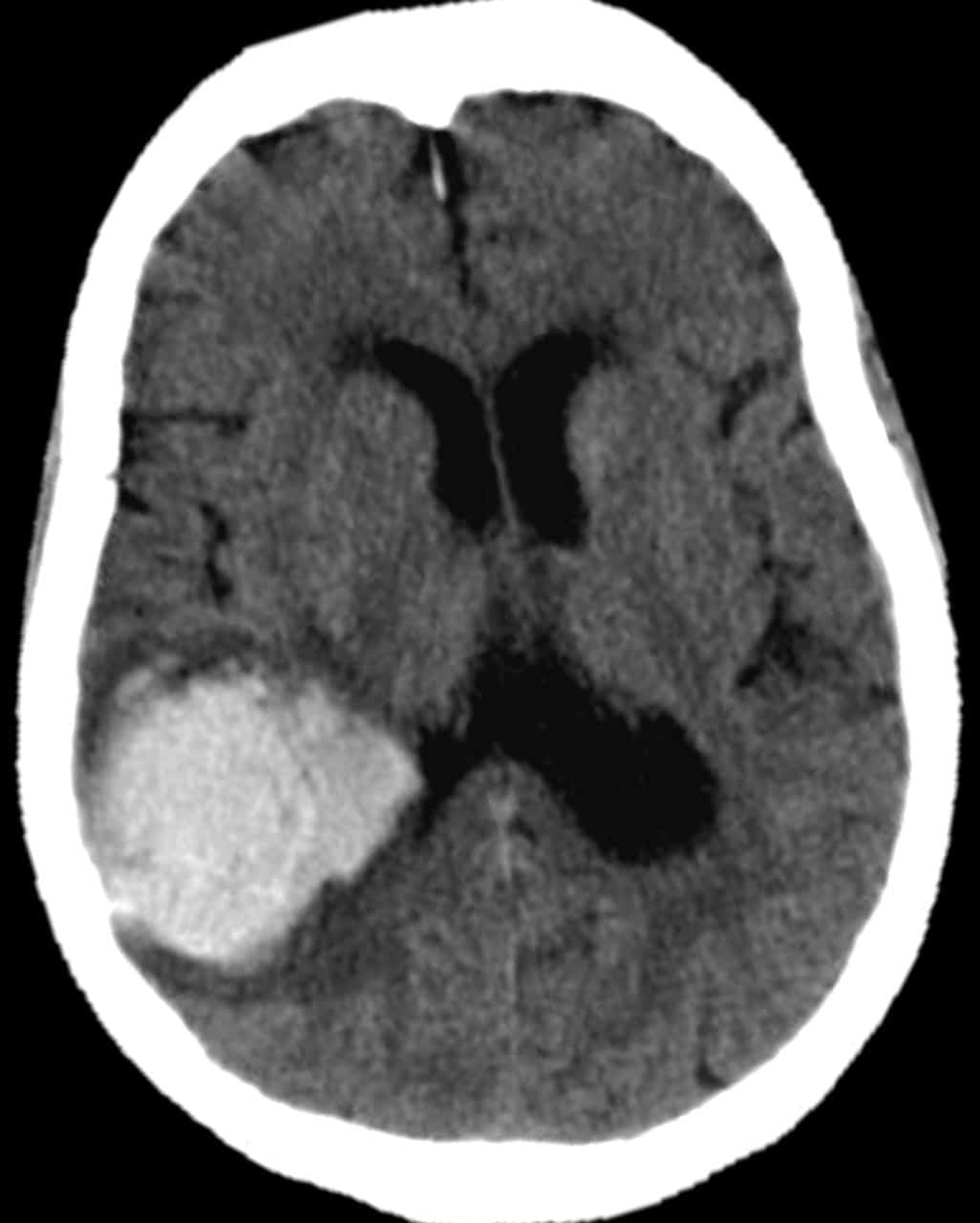
CT is the most widely used modality to rule out ICH. It also provides useful information on haematoma volume. Haematoma expansion usually occurs within the first 24 hours and is an independent predictor of increased mortality.
Repeat CT to evaluate haematoma expansion and oedema, is helpful especially if the patients neurological status deteriorates.
Investigation of the cause of the ICH is important as it may affect acute treatment and prognosis.
Patients who are <70yo and who have not had a hypertensive deep territory ICH, have a 1 in 4 to 1 in 7(depending on age) chance of an underlying vascular cause such as:
- Arteriovenous malformation
- Aneurysm
- Dural arteriovenous fistula
- Cavernoma
- Cerebral venous thrombosis
CTA and MRA have a >90%sensitivity and specificity for detecting vascular malformations.
Catheter intra-arterial DSA is the gold standard for determining the macrovascular cause with highest yield being for:
- Patients <70yo with lobar ICH
- <45yo with deep or posterior fossa ICH
- 45-70 yo with deep or posterior fossa ICH and no history of hypertension and no evidence of small vessel disease.
- All patients with ICH and CT r MRI evidence of macrovascular lesion
- IVH CT and MRI venography should be included.
Blood Pressure Control
Patients with acute ICH present with increased BP, which is associated with haematoma expansion, neurological deterioration and mortality.
Should we treat raised Blood Pressure? The results from major trials have been equivocal.
There are 2 major trials:
- INTERACT2 (Intensive Blood Pressure Reduction in Acute Cerebral Hemorrhage Trial)
- Increased SBP in the first 24 hours had a linear association with death at 90 days.
- Intravenous Nicardipine was used
- SBP reduction of > 20mm Hg in the first hour after randomisation and maintained for 7 days were associated with the lowest risk of death and major disability.
- ATACH-2 (Antihypertensive Treatment of Acute Cerebral Hemorrhage Trial)
- A range if IV agents were used
- Lowering SBP within 2 hours of ICH was associated with lower haematoma expansion and improved 90 day outcomes
- Allowed SBP to be decreased to 110-139, without increased mortality or worsened neurological outcomes.
A meta-analysis of both trials found that avoiding large fluctuations in BP is beneficial.
Studies have also shown that large reductions ie >60mmHg in the first hour was associated with worst outcomes. Therefore lowering the SBP too quickly should be avoided.
Smooth continuous lowering of blood pressure to a systolic blood pressure of 130-140mm Hg in acute ICH and SBP of 150-220mm Hg, is safe and may improve functional outcome.
Avoid lowering the SBP to < 130 mm Hg as it could be potentially harmful.
The BP lowering drug used should have a:
- Rapid onset
- Short duration
This allows better control and titration.
The RIGHT-2 (Rapid Intervention With Glyceryl Trinitrate in Hypertensive Stroke Trial), used transdermal nitroglycerine in ambulance, had worst outcomes with larger haematoma and oedema volumes. Venous vasodilators may be harmful due to unopposed venodilatation and its effects on haemostasis and ICP.
Haemostasis and Coagulopathy
Haemorrhage expansion and poor outcome is increased in patient with ICH on anticoagulation. Rapid reversal is required.
Anticoagulation
If the patient is on Warfarin (Vitamin K antagonist)
- 4 factor Prothombin complex concentrate is superior to plasma
- If INR is 1.3-1.9 give 10-20 IU/kg 4F PCC
- If INR > 1.9 give 25-50 IU/kg
- Give Vitamin K
If the patient is on a direct thrombin inhibitor ie., Dabigatran
- Use Idarucizumab
- If not available use 4 factor PCC
If the patient is on a Factor Xa inhibitor (Rivaroxaban, Apixaban etc)
- Use Andexanet alfa
- A recombinant coagulation factor reverses the inhibition of factor Xa
- Good haemostatic outcome, with a <35% increase in haematoma volume after 12 hours.
- If not available use 4 factor PCC
- At doses of 37.5-50 IU/kg 4 F PCC reversed coagulation assays.
Antiplatelet-related Haemorrhage
Antiplatelet therapy at time of haemorrhage has been associated with increased mortality and an unfavourable functional outcome.
There is no evidence that platelet transfusions, Desmopressin and TXA result in benefit to patients with ICH on antiplatelets.
One group which might benefit are those that are receiving an emergency craniotomy for haematoma removal. Platelet transfusion may reduce postoperative haemorrhage volume.
Complication Management
30% chance of developing a significant arrhythmia.
Older patient with large bleed ie >5cm had a higher likelihood of developing an arrhythmia. Most are in the first 24-72 hours.
Temperature Management
Fever in ICH is associated with increased clinical severity and worst outcomes. There is not great evidence that treating fever results in better outcomes.
Therapeutic hypothermia and other means of reducing temperature are a means of reducing perihaematoma oedema, however no clinical benefit has been demonstrated.
Seizures and Anti-seizure Medications
New onset seizures in ICH occur in about 28% of patients and tend to occur in the first 24 hours.
The benefit of prophylactic use of anti-seizure medication is unclear.
Small studies initially showed some benefit with Sodium Valproate and worst outcomes with Phenytoin
Recent studies have not shown consistent harm or benefit.
Non-invasive Monitoring, ICP/Oedema Management
Hyperosmolar therapy can be used to transiently reduce intracranial pressure, however the use of prophylactic hyperosmolar agents is uncertain.
Corticosteroids should not be administered for treatment of elevated ICP in ICH.