One of the exam favourites is to give you a picture. The idea is that it either gives a spot diagnosis, or forms the basis for a significant discussion.
When you think about this, don’t get too discouraged. In your career, you’ve seen most things. In the same way as there are only a finite type of ECG diagnoses, there are only a finite number of illustrations. The examiners love certain types of pictures. If you look at these few examples from past exams, its obvious that eyes are a favourite and if you look closely, so are necks.
Try the following examples and see what you can make of them.
Answer
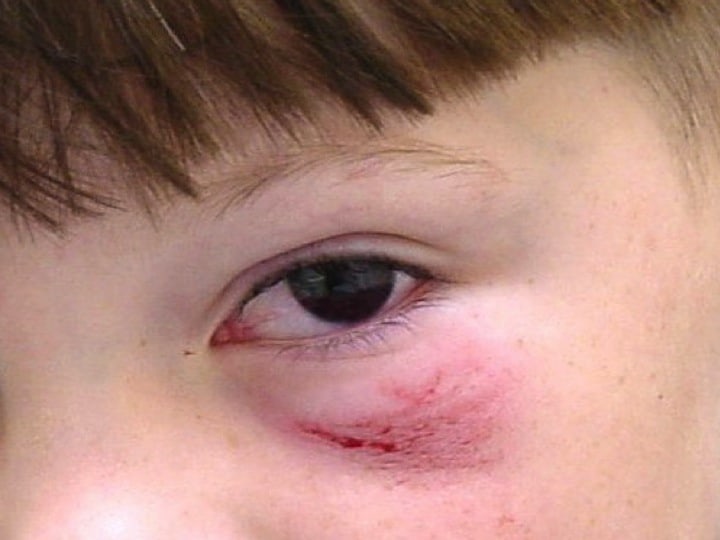
The obvious findings on the photograph are a hyphaema of approx 30%. There is also a partial ptosis of the lid and infra-orbital abrasions.We need to get a full history of how the injury occurred i.e.., what is the exact mechanism? We need to exclude other injuries. Traumatic hyphaemas are usually the result of projectiles, however the abrasion may not fit in with this story. This is a grade 2 hyphaema ie., 1/3-1/2.
The history should include:
-past history
-medications as well as
-immunisation status, as this is a potentially tetanus prone wound.
Examination should include:
-visual acuity as well as
-CN III, IV, VI, including
-afferent pupillary defect and
-slit lamp examination.
-Tonometry will also be needed as raised intra-occular pressure occurs in about 1/3 of cases, but beware of missing the globe rupture and if this is suspected, tonometry should not be performed.
Management is a shield over the eye, rest, analgesia and sitting at a 30-45 degree angle to hasten clearing of the eye and improvement of visual acuity.
Admission is indicated in this patient firstly because of the size of haematoma(certainly if there is any sickle cell trait) and secondly because there may be no-one available at home,which may be evidenced by the parents/carers not being present. The question needs to be raised as to why the parents are not present as the implication in the question, is that this injury occurred earlier in the day.
Interpretation
This photograph of good mouth opening(no real trismus) in a 12 year old. There is an obvious right mass that extends to the top of the oropharynx as well as crosses the midline and covers the uvula. There is no membrane or topical characteristics of infection. The mass crosses the midline such that swallowing may be difficult.The differentials given the mass and fever are quinsy, infectious mononucleosis, peritonsillar lymphoma.
Initial management must include assessment of airway, given the occlusive appearance of the lesion. However the photograph gives no indication of any distress(although it is a snapshot in time).
The patient should be in a high acuity cubicle (although not necessarily resus), with nasal cannula for oxygen delivery. Definitive treatment would include drainage of the quinsy. This can be done by ENT or in the emergency department.
Initial administration of dexamethazone early 8mg IV to rapidly reduce any swelling, as well as penicillin 1.2 g IV.
If there is any concern about the diagnosis I would consider investigating the lesion, by ultrasound first.
A quinsy of this size would require admission even if overnight.
Remember the parents, let them know what is happening, what you will do, get consent from the parents for a procedure.
Interpretation
The photo shows a male patient with swollen lips and some facial swelling. The patient does not appear to be in distress, although this picture is a snapshot in time and the patient has complained of difficulty breathing.
The likely diagnosis is angioedema, probably secondary to the ace inhibitor the patient is on, however an allergic reaction to the penicillin cannot be ruled out.
Initial management is in a high acuity area/resuscitation cubicle. It is important to find out how long ago the reaction began and if it is progressing or has stabilised.
The acute management of the patient would include:
- Resuscitation cubicle and non-invasive monitoring of heart rate, blood pressure and pulse oximetry.
- High flow oxygen is important to apply
- A focused past history related to previous episodes of this occurring, as well as other past medical history, including any history of airways disease is very relevant.
- Find out if the swelling is purely anterior in the lips and face or if the patient feels swelling in the back of the throat.
- Consider in the more compromised patient – nebulised adrenaline, intravenous access, IV dexamethazone
- Adrenaline may be given intramuscularly(IM) or intravenously(IV). The IM dose is 300-500mcg repeated every 5-10 minutes or IV 10-30mcg repeated every 5-10 minutes. For the sickest patients an infusion of adrenaline can be commenced.
- Be vigilant as airway compromise may occur in this type of patient.
- Consult with immunology re the reaction and with anaesthetics for assistance with airway. In a compromised airway, oral laryngoscopy will be difficult if there is also a swollen tongue. The alternatives are nasal intubation, or a surgical airway.
- Observe the patient potentially until the reaction has decreased and the concern of a rebound does not occur.
- Stop the offending medications.
- Post discharge, the patient may ned to followup for allergy testing.
ANGIOEDEMA
There are 3 different types of angioedema:
- Hereditary angioedema– also known as C1 inhibitor deficiency. It is due to increased kinins and urticaria is absent.
- Allergic angioedema– It is due to mast cell degranulation and urticaria is present.
- ACE inhibitor associated angioedema– Due to increased kinins and urticaria is absent.
The incidence of angioedema from enalapril is estimated at just over 1%, from findings in the OCTAVE trial(Am J Hypertens 2004;103-111). It can occur months to years after commencing the drug.
Can we predict who will develop angioedema?
The most significant risk factors are previous episode and African ancestry. Age and smoking and female gender are also risk factors although less significant. Diabetes decreases the risk(Hypertension 2008;51:1624-30).
Interpretation
This photo shows a male in bed with multiple burns of various depths. The burns are in the upper limbs as well as anterior torso. They also extend to the neck and there are facial burns. It is unclear if any of the burns are circumferential, however there is a significant airway risk here, with facial burns.
The patient has cardiac monitoring electrodes on and a hudson mask. There are covering over his arms which are assumed to be wet pads.
In respect to resuscitation of this patient, he needs a resuscitation cubicle, high flow oxygen and non-invasive monitoring including, pulse rate, blood pressure and oxygen saturations and then a rapid assessment of ABCD. It may be necessary to secure the airway if there are the classic hallmarks of inhalational injury which include, facial burns, singed nasal hair, soot in the upper airway, hoarseness, carbonaceous sputum and wheeze.
What constitutes a major burn?
- Partial thickness >25% body surface area(BSA) in 10-50 yo or 20% in <10/>50 yo
- Full thickness burns > 10%
- Burns with inhalational injury
- Burns to hands, feet and perineum
- Circumferential burns of an extremity (including neck).
- Burns crossing major joints or complicated by fractures or other trauma
- Electrical Burns
- Burns in high risk patients i.e. pregnant patient, extremes of age.
Fluid resuscitation is very important in the burns patient.
The classic teaching of the Parkland Formula which is mL of fluid = 4ml (3ml in children) x wt(kg) x % burns area. Half of this fluid should be given in the first 8 hours, the rest over 16 hours. Time starts at time of burn.
There are two main ways to calculate the burns area:
- Rule of 9’s- in the adult the head and arms are 9% each, the torso is 18% front and 18% back, the lower limbs are 18% each
- Lund and Browder Chart- more accurate
The patient in the photo has burns to the front of the torso, arms and head and therefore even with no other information we know that this is a major burn (rule of 9’s =9+9+9+18=45% at minimum). We can’t see the lower limbs and don’t know the weight of the patient. We can estimate weight of course. If these were the only injuries and this was the % BSA, then the Parkland formula tells us that the total fluid to be given is 4x45x80(kg)=14,400ml i.e. 14.4L of normal saline(most appropriate fluid to use), of which 7.2 L would need to be given over the first 8 hours. This is an estimate and the best way I believe to use the formula, so we have a picture of the sort of values of fluid we are going to need.
A better approach to fluid resuscitation, is to use empirical measures such as urine output, as more fluid may be needed. Aim for a urine output of 1-1.5mL/kg/hr.
Remember 2 large bore IV cannulas. This may be challenging depending on where the burns are.
Be careful with the fluids. I have often gone into a resus cubicle where a burns patient has been managed for several hours and they are borderline hypotensive and not producing much urine- FLUID, FLUID, FLUID and everything improves!
Other things to give and do.
Ensure there is adequate analgesia and that the patients tetanus status is known.
Cover burns area with sterile, saline soaked dressings but BEWARE or inducing hypothermia.
What about antibiotics?
There is no need for these in the resuscitation phase.
Who needs to go to a burns centre?
- Third degree burns of >5% in all patients
- Partial thickness burns >10% in adults
- In children partial/full thickness burns > 5%
- Inhalational injury
- Burn injury in <10 yo and > 50 yo
- Burns in children that require more qualified personnel to manage
- Burns to the face, hands, feet, genitalia, perineal region or major joint.
- Burn injury and trauma
- Burn injury and co-morbidities that could complicate management and recovery
- Electrical (including lightning), and chemical burns
A word on escharotomy
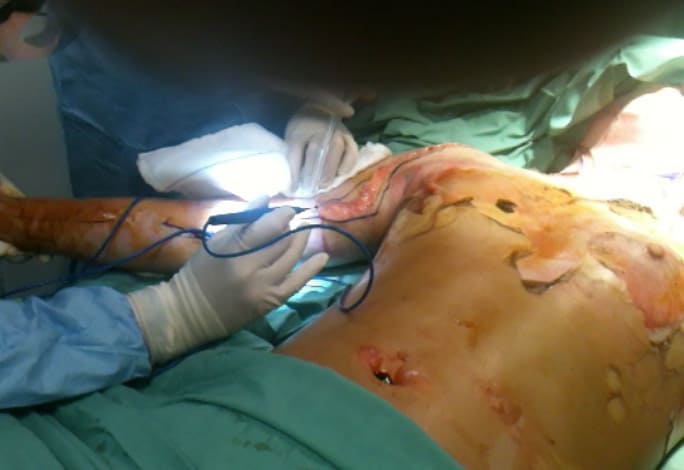
This is a required procedure when there are third degree burns that affect limbs neuromuscular status or can affect breathing when the chest is involved. A linear cut with scalpel or diathermy can be made on the limbs. On the chest a square division is made to separate the breast plate. This needs to be performed early, following airway and fluid resuscitation commencement.
Below is a picture of escharotomy on a major burns patient I saw a few years ago.
Interpretation
Interpretation
This is the ‘tomato sauce’ or ‘blood and thunder’ funds of central retinal vein occlusion. There are tortuous vessels and significant retinal haemorrhages.This causes a painless loss of monocular vision, that comes on over minutes. The patient can usually count fingers.
The cause of this condition is a restriction of blood leaving the retina.
Risk factors include; atherosclerosis, diabetes, hypertension, hyperviscocity syndromes and glaucoma.
Examination should also include slit lamp examination and examination for pupillary response.
There is no acute treatment for the condition and a proportion of patients retain useful vision. Complications such as glaucoma need to be aggressively treated as they can obviously affect outcome.
Interpretation
Interpretation
Hot bitumen burns are potentially terrible burns and removal of the bitumen is paramount as the burning continues whilst it is attached.This photo shows a child whose face we cannot see, but the image of the mouth may indicate distress. The soles of the feet are reddened and there is skin lifting and pustular formation over a significant area of the soles.The burns do not appear to be third degree burns.
Initial management must include continued local cooling and effective analgesia. This patient will need to be referred to an appropriate burns centre as one of the criteria for burns centre transfer i.e. “burns to face, hands feet, perineum or genitalia or major joint” has been met. Dressings will be in line with burns unit requirements, but clean non-occlusive dressings are appropriate.
Keep the parents involved at every part of this process, but be sure to get an adequate history and assess that it makes sense, so as not to miss any potential non-accidental injury. This can be further assessed outside the emergency department, given that this child will be admitted.
Interpretation
Interpretation
Interpretation
We need to say that right from the outset, that this will be a major injury. In children also beware of those that present with a high and low injury. There is a high chance that there will be an injury in the middle also.This photo shows abrasions along the whole lower back and flank area, with significant abrasions over the right flank. There is significant bruising over the buttocks especially the right buttock and there is perianal blood.
The potential injuries are huge in number. The assumption is that there has not been any head injury given the description of the injury for the photo and the fact that the child had a GCS of 15 on arrival.
If we look at the photo and align with what may be happening:
Skeletal injuries: Thoracolumbar spine, ribs , pelvis and femoral fractures are possible.
Solid organ injuries: Kidneys, liver and spleen lacerations as well as lungs contusions/lacerations, including haemothorax and pneumothorax.
Hollow organ injuries: Bowel rupture/laceration(large bowel and small bowel including duodenum), bladder perforation, cardiac contusions.
Vascular injury: aortic injury, IVC injury, multiple small vessel injuries dependant on organ and skeletal injury.










Pictures From The Fellowship Exam – Resus
[url=http://www.gjtkovns8uh69456b8fn722178yu495ts.org/]ujvjoqegtn[/url]
ajvjoqegtn
jvjoqegtn http://www.gjtkovns8uh69456b8fn722178yu495ts.org/