OK THRILL-SEEKERS, IT’S QUIZ TIME AGAIN!
Here are 3 visual questions for you.
The answers are below each question.
QUESTION 1
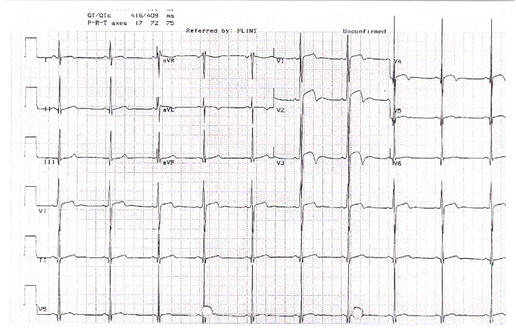
A 19 yo man is brought to the emergency department following a syncopal episode whilst playing basketball. His only history is of two previous episodes of syncope. The was no chest pain, no shortness of breath, no prodrome. He is waiting to be seen, but now wants to leave. The nurse shows you the ECG. What is the probable diagnosis that you must be concerned about?
ANSWER
Let’s analyse the ECG as we would in the ECG in 20 seconds approach:
The rate is 60bpm
It is sinus as each QRS is preceded by a P wave and they have normal morphology.
The QRS complex is narrow, and high in amplitude. It meets criteria for left ventricular hypertrophy. I use S in V1 + R in V5/6 > 35mm, or any R wave in limb lead > 20mm or in precordial lead >25mm. It’s important to note the deep narrow Q waves in the lateral leads V5/6. They are also present in the inferior leads. These are probably not infarct Q waves as they are too narrow. An infarct Q wave is usually > 1mm.
The ST-T segment is interesting in that there are depolarisation abnormalities. In fact in leads V2/3 there is an ST elevation pattern and a biphasic waveform that may be called Wellen’s syndrome, although it is not this.
Intervals: PR and QT are within normal limits.
This is the ECG of a probable hypertrophic cardiomyopathy. It has the high voltage QRS of left ventricular hypertrophy. Deep Q waves appear in lateral leads (also in inferior leads here which is not typical) and there are T wave changes and ST changes, which are probably the result of high voltages.
Given the presentation, this patient needs admission, monitoring and an echocardiogram.
QUESTION 2
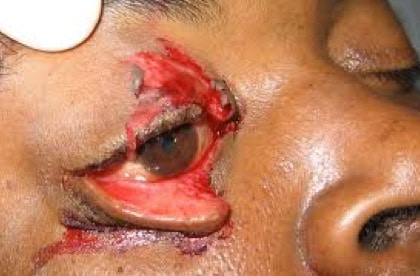
A 25 year old male is brought to the ED by ambulance. He tells you that he was punched repeatedly to the face, whilst just standing there, minding his own business.
You call the surgical registrar, who tells you to call plastics, who tells you to call opthalmology. The registrar tells you that there is no problem with you suturing this up as long as there is no damage to the eye itself(which there is not). “Surely you guys down there in the ED can handle that?” What will you use to get this repaired?
ANSWER
The phone, to call the opthalmology consultant, so he can take this patient to theatre. Why will you NOT suture this in the ED?
Beware all lacerations through the lid margins, any upper lid deep lacerations and any lacerations that may affect the medial one third of the eye and thus the lacrimal system. Now, having said all this, you must be able to describe the injury so the registrar knows what is going on on the end of the phone, because it’s not that easy to always picture.
QUESTION 3
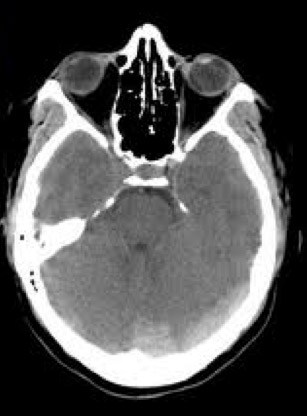
A 34 year old pregnant woman is brought to the ED by ambulance following a seizure. She is complaining of a headache. You perform a CT brain, shown below. What is the diagnosis?
ANSWER
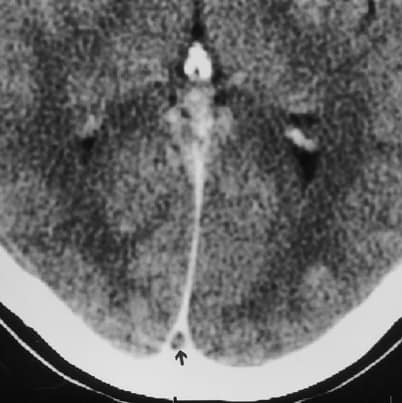
This patient has a venous sinus thrombosis, often called the DVT of the brain. It can result in headache, decreased GCS, seizures, stroke-like symptoms, and proptosis. In almost all cases papilloedema is present. Below is another classic sign- the ’empty delta sign’ in patients with superior sagittal sinus thrombosis.
I hope you enjoyed those. More to come. Let me know what you think.
Peter Kas