 Question 1 A mother brings her 2 year old child into the emergency department. She is distressed at the lesions that have appeared on her childs arms and are now spreading to his torso. They appeared 24 hours ago and are still there. The child is well looking, feeding well with normal vitals. The child has had a blocked nose and some viral symptoms over the last few days and the local doctor had commenced Amoxicillin.
Question 1 A mother brings her 2 year old child into the emergency department. She is distressed at the lesions that have appeared on her childs arms and are now spreading to his torso. They appeared 24 hours ago and are still there. The child is well looking, feeding well with normal vitals. The child has had a blocked nose and some viral symptoms over the last few days and the local doctor had commenced Amoxicillin.
What is your diagnosis? How might you manage the child/mother?
Answer
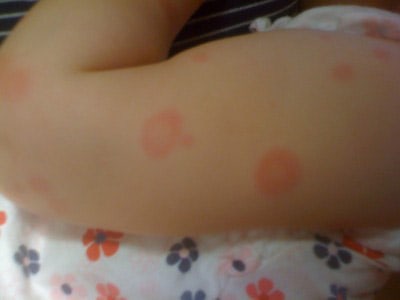
Erythema Multiforme. This is a self limiting hypersensitivity reaction, with very little(sometimes mild pruritis) prodrome. It can be caused by infections or by medication such as penicillins. The lesions, are symmetrical, begin in the extremities and spread proximally.
The classic target lesions take several days to appear and may have 3 distinct zones:
(a) central dark red area
(b) pink or oedematous zone
(c) peripheral red ring
The treatment here, especially if the child is well and has nothing more than minor oral mucosal involvement, is to stop the penicillin and review.
The Erythema Multiforme Blog is coming in the next week.
Question 2
 An 87 year old woman with a previous history of bowel cancer, presents to the emergency department with shortness of breath. Her saturations are 92% on 6L of oxygen via a Hudson mask.
An 87 year old woman with a previous history of bowel cancer, presents to the emergency department with shortness of breath. Her saturations are 92% on 6L of oxygen via a Hudson mask.
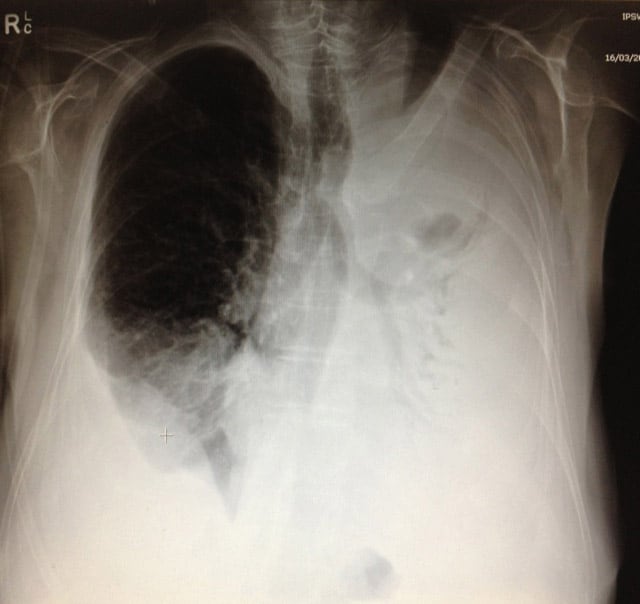
On auscultation there is stony dullness over the whole left lung. You perform a Chest X-ray. Describe the X-ray and give a diagnosis. How would you manage this patient?
Answer
There is obviously a large pleural effusion on the left. We can see air bronchogram. An air bronchogram is really an air-filled bronchus against surrounding opacified alveoli.
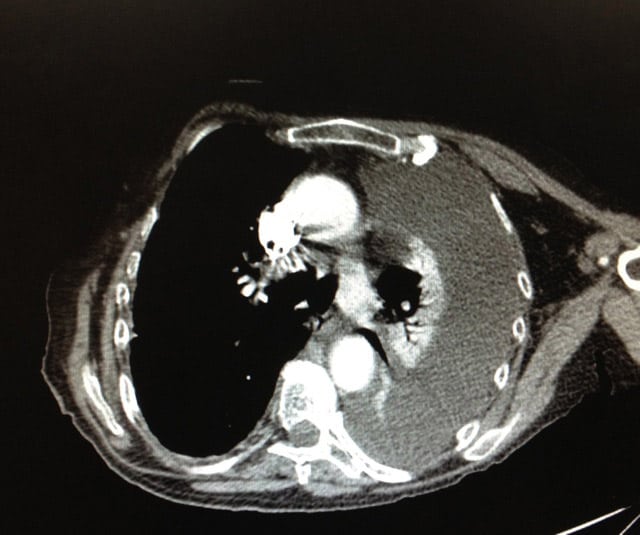 There was a concern in this patient about there being loculation, or where the lung started and ended. A CT was performed that demonstrated fluid and a collapsed lung.
There was a concern in this patient about there being loculation, or where the lung started and ended. A CT was performed that demonstrated fluid and a collapsed lung.
The management is can be as simple as a pleural tap. In this situation, the admitting unit requested an intercostal catheter, which given the size was not unreasonable.
Only 2L were removed with a good result.
Unlike ascitic taps, where up to 10L can be removed and albumin used to avoid circulatory dysfunction, in pleural taps no more than 2 L should be removed and some recommend no more than 1-1.5 L per day be the maximum. The reason for this is the risk of the rare, but well described re-expansion pulmonary oedema, that may occur(Ann Thorac Surg 1988:45;340-5).
 Question 3 A 30 year old male presents to the emergency department with central chest pain. He can only describe it as intense. It started gradually during the day. He has no previous medical history and no cardiac risk factors. His vitals are, heart rate of 98 bpm, afebrile and BP of 135/78, sats are 99% on room air and his respiratory rate is 18.
Question 3 A 30 year old male presents to the emergency department with central chest pain. He can only describe it as intense. It started gradually during the day. He has no previous medical history and no cardiac risk factors. His vitals are, heart rate of 98 bpm, afebrile and BP of 135/78, sats are 99% on room air and his respiratory rate is 18.
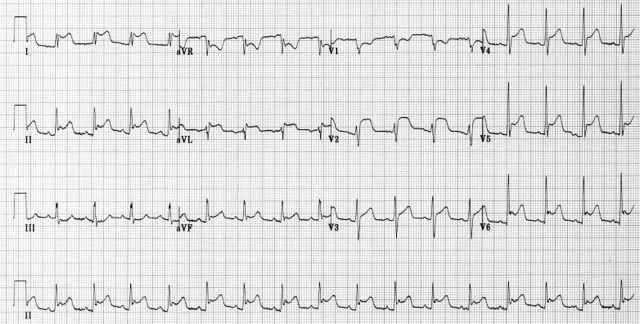
An ECG is performed. Please describe the ECG. What is your diagnosis?
What are the distinguishing features between an acute myocardial infarction, early depolarisation and acute pericarditis?
Answer
This is the ECG of acute pericarditis. Let’s look at the ECG using the ‘ECG in 20 seconds’ method.
Rate: 16 complexes x6 = 96bpm
Rhythm: There are p waves preceding every QRS, thus sinus. The P wave is also inverted in aVR and upright in II, indicating the limb leads are placed in the correct positions.
QRS: The QRS complex is narrow. It’s morphology is normal(ie., no delta waves) and the amplitude is normal.
ST-T Segments: There is widespread ST elevation (except for leads aVR and V1 and III). Apart from lead V2, it is concave in shape. There are no reciprocal changes. The ST/T ratio is > 0.25 in V6
PR/QT Intervals: The intervals are normal. However there is PR depression.
Comparing Features of AMI, Repolarisation and Pericarditis; here is a little table:
| AMI | EARLY REPOLARIZATION | PERICARDITIS | |
| ST Shape | Convex up | Concave up | Concave up |
| Location ST Elevation | Territory | Praecordial | Limb & Praecordial |
| Reciprocal ST charges | Yes | No | No |
| Q waves | Yes | No | No |
| Loss R wave voltage | Yes | No | No |
| PR depression | No | No | Yes |
| ST/T ratio in V6 | N/A | <0.25 | >0.25 |
(Adapted from Am Fam Physician 1998 Feb)
Peter Kas









