Here is the case
You have a 24 year old, right-handed tradesman, with who fell over playing football on the weekend. He has injured his right wrist, he has tenderness over distal radius and snuff box and his initial x-ray series is normal. What next?
This blog contains the short answers, and the longer answers for those who want to look at the topic in more detail.
Clinical examination and plain x-rays are known to be poor at identifying scaphoid fractures immediately after the injury. Retrospective studies suggest that 10-33% of patients with a proven fractured scaphoid had no fracture visible on the initial plain x-rays,
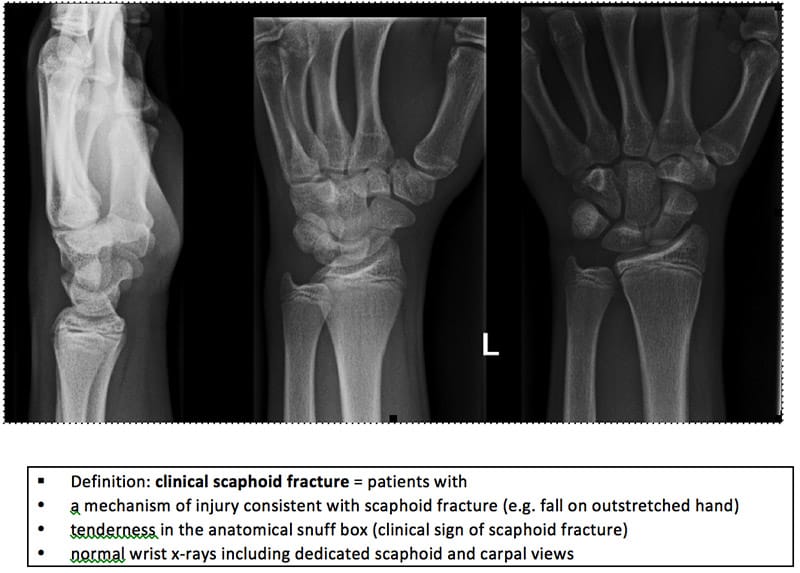
The x-ray below demonstrates a scaphoid fracture.
This blog is not aimed at the management of particular scaphoid fractures. The evidence is not convincing for any particular approach, and seeking an opinion from your local orthopaedic surgeon for conservative versus operative management seems like a reasonable approach.
In patients with clinical findings suggestive of fractured scaphoid, and normal scaphoid views, traditional practice was to immobilise in plaster for 10 days before a repeat clinical examination and plain x-ray3 This practice has evolved to minimise the risk of long-term morbidity associated with missed fracture of scaphoid: osteoarthritis of the wrist, long-term functional disability and chronic pain
It is also known that relatively few 2-15% of patients immobilised will subsequently be shown to have a fracture. Therefore many patients are unnecessarily immobilised. This is a condition that typically afflicts young active patients8 and may incur a significant cost to the individual and community in terms of lost working days. Furthermore, prolonged plaster immobilisation and activity restriction can result in a significant loss of bone mineral and muscle mass in a few weeks.
Over the last two decades, the development of newer medical imaging technology has prompted researchers and clinicians to explore better ways of diagnosis. There is a reasonable body of evidence published on new medical imaging technology and applications. The mostly small studies in the literature advocate various diagnostic options.
- Plaster immobilisation and repeat examination & x-rays in 10 days,
- Bone Scan (Day 4 or Day 10)
- MRI (early or Day 10),
- CT
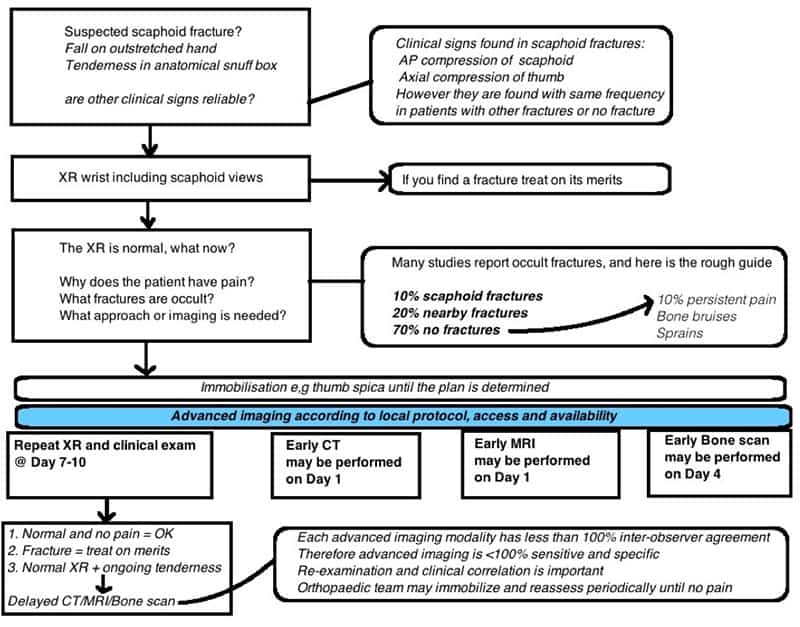
Here is an algorithm that tries to capture on one page, a rational diagnostic approach
Want more detail?
The studies discussed below were conducted on patients the same or similar to our definition of clinical scaphoid fracture. Unfortunately the use of ‘reference standards’ varies, with the various imaging modalities used as each other’s reference standard in a fashion that has evolved over time. Essentially delayed radiographs have been gradually replaced by advanced imaging, in particular MRI. The issue of new, more advanced technologies detecting more injuries has been dealt with by either calling them “false positives” compared to the existing reference standard, or by claiming the new test is now the new “gold standard”, because it detects additional injuries. The significance of such injuries has not been well evaluated in terms of patient outcomes.
The literature highlights the strengths and limitations of using early advanced medical imaging. Certainly for scaphoid and carpal fractures, introduction of new medical imaging technology has resulted in diagnosis of fractures that were not evident on the initial x-rays. This has resulted in the evolution of what is defined as the reference standard test for diagnosis of scaphoid fracture. MRI is considered the gold standard by the American College of Radiologists.
CT
- Initially there were multiple small studies published
- Larger studies show very good sensitivity and specificity
- Interobsever agreement is less than 100%
For example Breederveld investigated the validity of CT scanning and bone scan compared with the clinical fracture rate during follow-up of 1 year for examining patients with a suspected scaphoid fracture. The sensitivity, specificity, and positive and negative predictive values of the CT scan were 100%. The sensitivity, specificity, and positive and negative predictive values of bone scan were 78%, 90%, 78%, and 90%, respectively. However the tests were performed 5 to ten days after injury, at which time fracture healing might be present, thus the performance may be different to performance on the day of injury
More recent study showed CT had substantial intraobserver and interobserver reliability for the diagnosis of a nondisplaced scaphoid fracture. N = 180 (six observers) (17fractures & 13 normal) The average sensitivity, specificity, and accuracy of CT for a nondisplaced scaphoid fracture were 89%, 91%, and 90% for the first round and 97%, 85%, and 88% for the second round of observations, respectively.
The author of this blog (Cruickshank et al) published/presented the following:
Early CT is accurate in the diagnosis of scaphoid fractures.
- Sensitivity = 94%
- Specificity = 100%
- Negative predictive Value = 96.7%
- Positive Predictive Value = 100%
Early CT in a clinical practise guideline is useful.
- Sensitivity = 100%
- Specificity = 100%
- Negative predictive Value = 100%
- Positive Predictive Value = 100%
- Days in plaster mean 2.9, median 0, range 0-56
- Time off work mean 1.6 days, median 0, range 0-14
- Patient satisfaction 4.2/5
CT is reliable and precise, with excellent interobserver reliability of radiologist interpretation of CT
- Kappa (scaphoid fracture) = 0.88
- Kappa (all fractures) = 0.5
Magnetic Resonance Imaging (MRI)
- MRI provides high quality images, with no ionizing radiation exposure to the patient
- MRI identifies new fractures and soft tissue injuries
- MRI is not 100% specific, and has less than 100% interobserver agreement
- · MRI is now regarded by many as the gold standard for the imaging of scaphoid fractures in cases in which the initial radiographs are normal.
So MRI is great, right? no controversy? Let’s see.
Role of MRI in the diagnosis and management of patients with clinical scaphoid fracture
Methods
A consecutive series of 137 patients referred to the orthopaedic department with clinically suspected scaphoid fracture but normal series of plain radiographs were prospectively followed up over a two-year period. We implemented the use of early MRI for these patients and determined its incidence of detected scaphoid injury in addition to other occult injuries. We then prospectively examined results of these findings on patient management.
Results
Thirty-seven (27%) MRI examinations were normal with no evidence of a bony or soft-tissue injury. Soft-tissue injury was diagnosed in 59 patients (43.4%). Of those, 46 were triangular fibrocartilage complex (TFCC) tears (33.8%) and 18 were intercarpal ligament injuries (13.2 %). Bone marrow oedema with no distinct fracture was discovered in 55 cases (40.4%). In 17 (12.5%) cases, this involved only the scaphoid. In the remainder, it also involved the other carpal bones or distal radius. Fracture(s) were diagnosed on 30 examinations (22.0%).
Conclusions
MRI should be regarded as the gold standard investigation for patients in whom a scaphoid fracture is suspected clinically. It allows the diagnosis of occult bony and soft-tissue injuries that can present clinically as a scaphoid fracture; it also helps exclude patients with no fracture. We believe that there is a need to implement national guidelines for managing occult scaphoid fractures.
This recent paper highlights that MRI by detecting injuries can be declared the new gold standard, but it does not actually compare this gold standard to an existing gold standard, or to another test, and it also does not address the issue of inter-observer agreement. If we just read the abstract without further questions, then that can be a problem. Perhaps look no further than another article published in the same year
MRI as a reference standard for suspected scaphoid fractures
Methods
In a prospective study, 33 healthy volunteers were recruited and both wrists of each were scanned, except for 2 volunteers for whom only one wrist was scanned. To simulate the usual clinical context the 64 scans of healthy volunteers were mixed with 60 MRI scans of clinically suspected scaphoid fractures but normal scaphoid radiographs. These 124 MRI scans were blinded and randomly ordered. Five radiologists evaluated the MRI scans independently for the presence or absence of a scaphoid fracture and other injuries according to a standard protocol.
Results
To answer the primary question, only the diagnoses from the 64 scans of healthy volunteers were used. The radiologists diagnosed a total of 13 scaphoid fractures; therefore, specificity for diagnosis of scaphoid fracture was 96% (95% confidence interval: range 94–98%). The 5 observers had a moderate interobserver agreement regarding diagnosis of scaphoid fracture in healthy volunteers (multirater κ=0.44; p<0.001).
Conclusions
The specificity of MRI for scaphoid fractures is high (96%), but false-positives do occur. Radiologists have only moderate agreement when interpreting MRI scans from healthy volunteers. MRI is not an adequate reference standard for true fractures among patients with suspected scaphoid fractures.
So, even gold standards are prone to false positives and less than perfect inter-observer agreement. In terms of critical evaluation of MRI as the current gold standard for diagnosis of scaphoid fractures, it is worth noting some of the less disputable facts.
- Demonstrated accurate diagnosis of scaphoid and other nearby fractures, with reported 100% negative predictive value, sensitivity and specificity.
- MRI is also highly reliable and precise with kappa values of 0.8-0.95.
- MRI is very sensitive at detecting bone marrow oedema, a change which cannot be seen immediately with other radiological techniques.
- It is now well documented that patients with clinical scaphoid fracture, have not only scaphoid fractures but other fractures demonstrated on MRI. These other injuries include fractures to any of the nearby bones in the distal forearm, wrist and carpals, and hand.
- The prevalence of scaphoid fracture ranges from 13 19% , and other fractures collectively from19%to 24% . This leaves approximately two thirds of patients with no demonstrable fracture (range 62%- 64%)
However, there are some inconsistencies in conclusions drawn from the evidence (see boxes below)
- The significance of the MRI finding of bone marrow oedema, a bone bruise: without fracture, following trauma to the scaphoid has been debated, with recent evidence that it is a benign injury and is unlikely to result in long-term morbidity in the form of non-union..
- A definition of fracture has normally been a disruption of the cortex (edge) or trabecular pattern (within the bone). There is evidence to suggest that MRI is superior in detecting trabecular fractures than CT, but CT is superior in detecting cortical fractures.
- Kappa is only reported between pairs of observers – extrapolation of these results to other radiologists should be done with caution.
- When advanced medical imaging depicts fractures not evident on the existing reference standard, it is inappropriate for authors to suggest that bone scan is prone to “false positives” when it suggests a fracture that is not evident on delayed x-rays, but to then declare that MRI detects fractures not evident on plain x-ray and is thus more accurate than delayed x-rays.
See what you think of this… (who really likes letters to the editor about your research?)
The incidence of MRI detected scaphoid and other wrist fractures was determined in a clinical setting in patients with suspicion of scaphoid injury and negative initial radiographs…195 patients were scanned. There were 37 scaphoid fractures (19%), 28 distal radius fractures (14%), 9 fractures of other carpal bones (5%) and 119 studies with no fracture. The management of 180 patients (92%) was altered as a result of the MRI scan… MRI allows an early definitive diagnosis to be made, changing patient management in over 90% of cases and should be regarded as the gold standard investigation in this population.
Gold—now you see it, now you don’t
The Editor—Sir,
Drs Brydie and Raby make a compelling argument for the valueof early MRI in the management of scaphoid fractures. However,their discussion of diagnostic “gold standards” in this conditionwould do credit to a street magician. They point out that for investigating clinical scaphoid fractures,”plain radiographs [including delayed films] have been the goldstandard to date”. However, they do not tell us how many oftheir 195 patients in whom a clinical scaphoid fracture wasnot visible on initial radiographs, delayed radiographs actuallyconfirmed the diagnosis, i.e. how many of the MRI positiveswere confirmed by the existing gold standard? We are not giventhe number of the false positive MRIs, nor the number of falsenegatives, relative to what the authors have stated is the “existinggold standard”.In discussion, the authors point out that bone scintigraphyhas “high sensitivity for fracture, but poor specificity witha false positive rate of 25% when compared with delayed radiographs”.How does it come about that when the radionuclide procedureis more sensitive than delayed radiographs, it is because offalse positive nuclear medicine studies, whilst when MRI ismore sensitive (probably – although data weren’t includedin the authors’ paper) the argument is that the apparently moresensitive test should become the new gold standard? A more balanced view would strengthen the authors’ case.
Bone Scan
There is evidence to support bone scan on day 4 post injury, with excellent sensitivity and negative predictive values (95-100%), although the specificity (60-95%) and positive predictive value (65%) represent a limitation of the test. Although not calculated in the publication, the confidence intervals in Murphy’s study would be quite good.
Interobserver reliability and intraobserver reliability was shown to be reasonable however there was episodes of disagreement by a panel of experts.
A more recent study involved implementation of bone scan in an acute setting. Bone scan was performed no earlier than 72 hours post injury, if the patient has suspected scaphoid fracture (swollen and tender anatomical snuff box) and normal initial x-rays.13 Bone scan was used to determine definitive treatment, in a similar design to our 2nd scaphoid project using CT. Fractures were confirmed by the orthopaedic clinic rather than using another test, and all patients were followed up at three months – one patient with no fracture had minor discomfort, and therefore it was assumed no significant fractures were missed. While this study has some limitations in terms of the reference standard, it appears to provide reasonable evidence for the effectiveness of bone scan in practice.
Interobserver reliability, “precision of tests”
One measure of performance of a test is the precision, or reproducibility of results. Studies on MRI have documented good observer agreement (kappa>0.810, kappa 0.95). Thorpe demonstrated MRI had superior IOR to Bone scan. IOR for bone scan was reported as 0.57, 0.81 for static phase. One study compared agreement of six observers between displaced vs non displaced fractures on CT.Intraobserver reliability for CT interpretation is excellent with K=0.79 (95%CI 0.73-0.83). Interobserver reliability is substantial over two groups of measurements with K=0.62-0.70.
The study by Cruickshank et al was presented but not published Itdemonstrates good interobserver reliability for scaphoid fractures, with less agreement for other fractures. It examined interobserver reliability using nine radiologists. This is the largest group in the literature.
The results were obtained using a sample of 135 observations, and by using nine radiologists introduce more potential for variability in reporting, which should ensure our results relevant to a broad audience.
Kappa represents average agreement between observers, and as such can be influenced by outlier results. In the study, one individual reported substantially more fractures than the other radiologists, and this resulted in one person having a disproportionate affect on the level of agreement. It is also interesting that certain radiological findings were associated with disagreement between radiologists. Two patients in particular had findings that caused disagreement. Many studies of CT and MRI demonstrate a range of fractures in patients presenting with clinical scaphoid fracture, and that these injuries should be considered when reporting CT.
Clinical Practice Guidelines
Guess what?
- Guidelines are not often used,
- The recommendations in the published guidelines vary between local sites.
Further detail below
International use of scaphoid guidelines by institutions/departments.
An international survey of scaphoid imaging protocols and practice revealed marked inconsistency in imaging of acute scaphoid injury. Only 23 of 105 hospitals had fixed protocols, and the results below highlight that despite a lack of protocols, current practise was “known”, and that current practise is diverse.
Before second-line investigations were initiated, repeat x-rays were usually performed in 76 of the 105 hospitals. In 29 hospitals, other imaging techniques were used without further x-rays.
Second line investigations varied:
- MRI in 31/105,
- CT in 19/105, and
- Bone scan in 14/105.
- CT or MRI in 10/105,
- CT or bone scan in 6/105,
- Bone scan or MRI in 6/105,
- CT then MRI (if CT was negative) in 1/105,
- both CT and bone scan in 1/105, and
- bone scan then CT (if positive) in 1/105.
- Equal preference among MRI, CT, and scintigraphy in 10/105
- Clinical examination and radiographs were used alone in 6/105.
Knowledge of scaphoid guidelines. (British ED staff)
A second study involved assessment of knowledge of clinicians in the Emergency Departments in England & Wales to evaluate the current trend for the acute management of radiologically normal, but clinically suspected, fractures of the scaphoid.
A survey of 146 A&E senior house officers (SHOs) in 50 different hospitals
- The majority (55.8%) of SHOs performed only one test to diagnose suspected scaphoid fractures.
- A minority had reasonable knowledge of appropriate diagnosis and management.
- 54% not aware of local guidelines for the management of suspected scaphoid fractures
- 92% not aware of the existence of the 1992 British Association for Accident and Emergency Medicine (BAEM) guidelines.
The authors suggest that clinical knowledge and the management of suspected scaphoid fractures in A&E are unsatisfactory, and also suggest that the dissemination of up-to-date guidelines could help to educate clinicians to provide better care to the patients. A search of the BAEM website reveals that the current guideline is under revision, and not publicly accessible. In terms of diagnosis of suspected scaphoid fracture, In Australia there are no guidelines on the website of the Australasian College for Emergency Medicine, Australasian College of Radiologists, or Royal Australasian College for Surgeons.
The American College of Radiologists has a guideline, which can be found using the following link
Reference list
Murphy DG, Eisenhauer MA, Powe J, Pavlofsky W. Can a day 4 bone scan accurately determine the presence or absence of scaphoid fracture? Annals of emergency medicine. 1995; 26: 434-8.
Kusano N, Churei Y, Shiraishi E, Kusano T. Diagnosis of occult carpal scaphoid fracture: a comparison of magnetic resonance imaging and computed tomography techniques. Techniques in hand & upper extremity surgery. 2002; 6: 119-23.
Munk B, Frokjaer J, Larsen CF, et al. Diagnosis of scaphoid fractures. A prospective multicenter study of 1,052 patients with 160 fractures. Acta orthopaedica Scandinavica. 1995; 66: 359-60.
Krasin E, Goldwirth M, Gold A, Goodwin DR. Review of the current methods in the diagnosis and treatment of scaphoid fractures. Postgraduate medical journal. 2001; 77: 235-7.
Perron AD, Brady WJ, Keats TE, Hersh RE. Orthopedic pitfalls in the ED: scaphoid fracture. The American journal of emergency medicine. 2001; 19: 310-6.
Waizenegger M, Wastie ML, Barton NJ, Davis TR. Scintigraphy in the evaluation of the “clinical” scaphoid fracture. Journal of hand surgery (Edinburgh, Scotland). 1994; 19: 750-3.
Murphy D, Eisenhauer M. The utility of a bone scan in the diagnosis of clinical scaphoid fracture. The Journal of emergency medicine. 1994; 12: 709-12.
[Ring D, Jupiter JB, Herndon JH. Acute fractures of the scaphoid. The Journal of the American Academy of Orthopaedic Surgeons. 2000; 8: 225-31.Pillai A, Jain M. Management of clinical fractures of the scaphoid: results of an audit and literature review. Eur J Emerg Med. 2005; 12: 47-51.
Brydie A, Raby N. Early MRI in the management of clinical scaphoid fracture. Br J Radiol. 2003; 76: 296-300.
Bretlau T, Christensen OM, Edstrom P, Thomsen HS, Lausten GS. Diagnosis of scaphoid fracture and dedicated extremity MRI. Acta orthopaedica Scandinavica. 1999; 70: 504-8
Breederveld RS, Tuinebreijer WE. Investigation of computed tomographic scan concurrent criterion validity in doubtful scaphoid fracture of the wrist. The Journal of trauma. 2004; 57: 851-4.
Cruickshank J, Meakin A, Breadmore R, et al. Early computerized tomography accurately determines the presence or absence of scaphoid and other fractures. Emerg Med Australas. 2007; 19: 223-8.
Brydie A, Raby N. Authors’ reply. Br J Radiol. 2003; 76: 923-a-24.
Robinson P. Gold–now you see it, now you don’t. Br J Radiol. 2003; 76: 923-.
Trigg M, Reeves PJ. The efficacy of plain films vs MRI in the detection of scaphoid fractures. Radiography. 2007; 13: 56-64.
Tai CC, Ramachandran M, McDermott ID, Ridgeway S, Mirza Z. Management of suspected scaphoid fractures in accident and emergency departments–time for new guidelines. Annals of the Royal College of Surgeons of England. 2005; 87: 353-7.
Groves AM, Kayani I, Syed R, et al. An international survey of hospital practice in the imaging of acute scaphoid trauma. Ajr. 2006; 187: 1453-6..
Brondum V, Larsen CF, Skov O. Fracture of the carpal scaphoid: frequency and distribution in a well-defined population. European Journal of Radiology. 1992; 15: 118-22.
Kumar S, O’Connor A, Despois M, Galloway H. Use of early magnetic resonance imaging in the diagnosis of occult scaphoid fractures: the CAST Study (Canberra Area Scaphoid Trial). New Zealand Medical Journal. 2005; 118: U1296.
La Hei N, McFadyen I, Brock M, Field J. Scaphoid bone bruising–probably not the precursor of asymptomatic non-union of the scaphoid. The Journal of hand surgery, European volume. 2007; 32: 337-40.
Raby N. Magnetic resonance imaging of suspected scaphoid fractures using a low field dedicated extremity MR system. Clinical radiology. 2001; 56: 316-20.
Buul MMC, Beek EJR, Dongen A, Royen EA. The reliability of the 3-phase bone scan in suspected scaphoid fracture: an inter- and intraobserver variability analysis. European Journal of Nuclear Medicine and Molecular Imaging. 1992; 19: 848-52.
Beeres FJ, Hogervorst M, Den Hollander P, Rhemrev SJ. Diagnostic strategy for suspected scaphoid fractures in the presence of other fractures in the carpal region. Journal of Hand Surgery – British Volume. 2006; 31: 416-8.
Akdemir UO, Atasever T, Sipahiolu S, Turkolmez S, Kazimolu C, Sener E. Value of bone scintigraphy in patients with carpal trauma. Annals of Nuclear Medicine. 2004; 18: 495-9.
Tiel-van Buul MM, Broekhuizen TH, van Beek EJ, Bossuyt PM. Choosing a strategy for the diagnostic management of suspected scaphoid fracture: a cost-effectiveness analysis.[see comment]. Journal of Nuclear Medicine. 1995; 36: 45-8.
Beeres FJ, Hogervorst M, den Hollander P, Rhemrev S. Outcome of routine bone scintigraphy in suspected scaphoid fractures. Injury. 2005; 36: 1233-6.
Adey L, Souer JS, Lozano-Calderon S, Palmer W, Lee SG, Ring D. Computed tomography of suspected scaphoid fractures. The Journal of hand surgery. 2007; 32: 61-6.
Thorpe AP, Murray AD, Smith FW, Ferguson J. Clinically suspected scaphoid fracture: a comparison of magnetic resonance imaging and bone scintigraphy. Br J Radiol. 1996; 69: 109-13.
N’Dow J, N’Dow K, Maffulli N, Page G. The suspected scaphoid fracture. How useful is a unit policy? Bulletin of the Hospital for Joint Diseases. 1998; 57: 93-5.
Grimshaw JM, Russell IT. Effect of clinical guidelines on medical practice: a systematic review of rigorous evaluations. The Lancet. 1993; 342: 1317-22.
by Jaycen Cruickshank – Jaycen is a new member of the team. He is the Director of Emergency at Ballarat Health Services and has an interest in, as well as having published on this topic.










Diagnosis of Scaphoid Fractures – Resus
hwzebofo http://www.gw8b136mm3137drrn8zvue9338936hyhs.org/
[url=http://www.gw8b136mm3137drrn8zvue9338936hyhs.org/]uhwzebofo[/url]
ahwzebofo
スーパーコピーブランド
airport fence factory
Active Harmonic Filter
スーパーコピーブランド
LouisVuittonルイヴィトンベルト販売店
Cookie Containers
Bvlgariブルガリ時計コピー
Two Piece
Vintage Windows
Bvlgariブルガリブレスレット販売店
StellaMccartneyステラマッカートニーコピー激安
Auto Ac Compressor For Nissan
Cartierカルティエブレスレットコピー
Moving Head Stage Lights
Cold Green Tea
ブランドBvlgariブルガリ時計コピーN級品
WSPE/F
Gucciグッチバッグコピー
Cost Of Submersible Water Pump Supplier
Gucciグッチ指輪販売店
Balenciagaバレンシアガブランドコピー代引き
Massage Furniture
Twin Screw Extruders & Calenders
ブランドChanelシャネルバッグコピーN級品
StellaMccartneyステラマッカートニー財布コピー
22 Toro Recycler Lawn Mower Blade
ブランドLouisVuittonルイヴィトンスマホケースコピー代引き
Aluminum Silencer Accessories
ブランドコピー代引き
Linak Electric Hospital Bed
ブランドコピー専門店
Side Tables Decor
Polyurethane Silicone Sealant
ブランド時計コピー
コピー時計
Flossing Teeth At Home
12305-40110
Polymeric
ブランド時計コピー
10HP 400F 7.5KW Crusher
Compostable Plastic Bags
ブランドバッグコピー
PU Pacifier Cord Chain
スーパーコピーバッグ
Automatic Robotic Vacuum Cleaner
Fuel Injectors for Mazda