A 25 year old male presents to the emergency department following a near syncopal episode. His ECG shows a supraventricular tachycardia(SVT). Vagal manoeuvres are attempted, unsuccessfully. Adenosine is then given for reversion. He reverts and his post-reversion ECG is shown below. One of the registrars is concerned that the ECG is showing a Brugada pattern.
Is this right? Is this a Brugada Pattern and has the patient demonstrated Brugada Syndrome? Do patients with Brugada even present with an SVT?
How do we make the diagnosis and what do we look for in the ECG? Brugada is one of the ECG’s of Syncope, that we cover in the Cardiac Bootcamp.
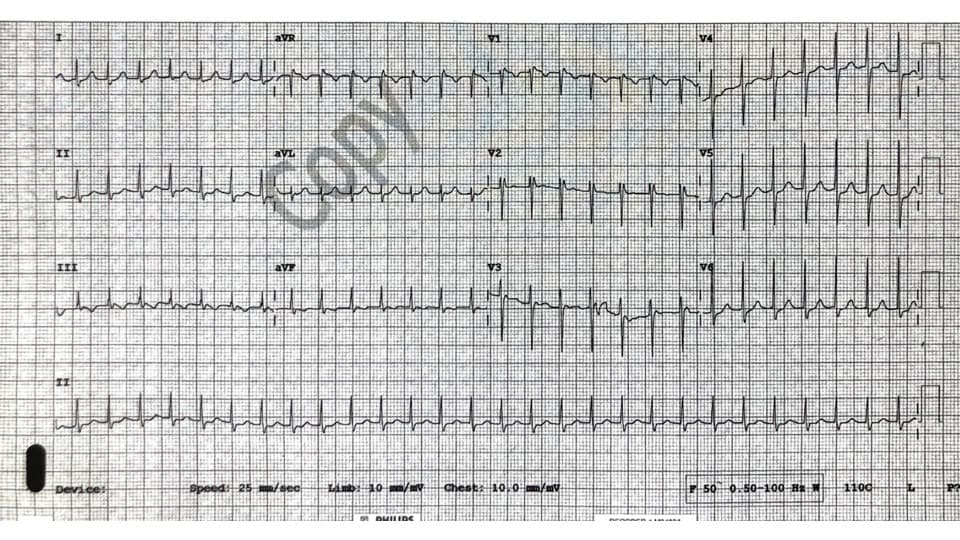
SVT in patient with pre-syncope
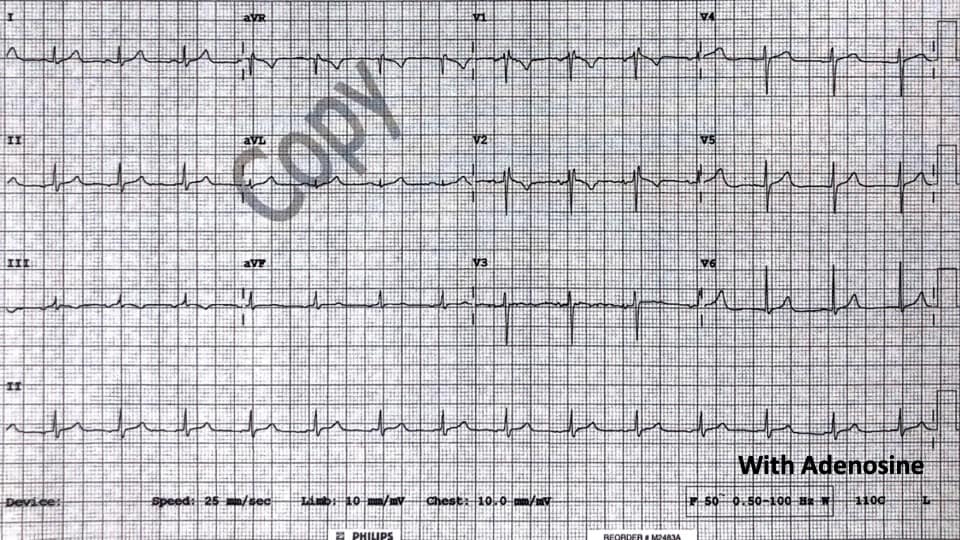
Post Adenosine
What is Brugada Syndrome?
It is an inherited autosomal dominant Na+ channel abnormality(1). It is far more common in males (by factor of 8-10:1) where it is the second most common cause of death in those less than 40 years of age. The true prevalence is difficult to estimate, as it is a dynamic ECG pattern, ie., it is not always present. It is usually associated with sudden death in those with structurally normal hearts.
It’s prevalence is about 5/10000 of the population, being responsible for approximately 4% of all sudden cardiac deaths. It has a high prevalence in South-East Asia and is the same disorder as the previously known Sudden Unexplained Nocturnal Death Syndrome(SUNDS)(2)
Patients may suffer sudden cardiac death, or present in cardiac arrest, usually with polymorphic ventricular tachycardia or ventricular fibrillation(VF) being the most common arrhythmias. Patients with the syndrome, may also present following a syncopal episode, which may be a result of self-termination of the arrhythmia.
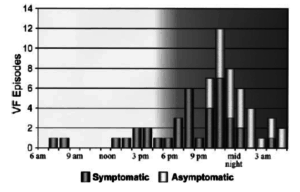 Beware the patient whose partner or family member describe nocturnal agonal respirations, as VF and sudden death in Brugada usually occurs at night or at rest(2). This may be due to sympathovagal balance or bradycardia which may initiate the arrhythmia.
Beware the patient whose partner or family member describe nocturnal agonal respirations, as VF and sudden death in Brugada usually occurs at night or at rest(2). This may be due to sympathovagal balance or bradycardia which may initiate the arrhythmia.
The high prevalence in Asian populations has seen specific language emerge to describe it’s occurrence at night(3):
- In Thailand, ‘Lai Tai’ was the term used to describe nocturnal deaths. The word “Lai” means a loud groan occurring in sleep and “Tai” means death.
- In the Philippines Bangungut, means “to rise and moan in sleep,” and describes the disease.
- In Japan, Pokkuri Death Syndrome, was similar, with “Pokkuri” meaning sudden, unexpected death.
Making the Diagnosis
The diagnosis is made when both:
- The diagnostic Brugada ECG pattern is present and
- There is a relevant clinical history.
ECG Findings in Brugada Syndrome
The changes seen on ECG, known as the Brugada pattern may be concealed, intermittent or dynamic, probably secondary to the Na+ channel dysfunction being affected by several factors.
The pattern is more likely to be seen in the following circumstances:
- Fever
- Intoxication
- Vagal Stimulation
- Electrolyte abnormality ; hyper/hypo K+, hyperCa2+
- Unmasked by Na+ channel blockers
- Medication related:
- Alpha agonists
- Beta blockers
- Tricyclic/tetracyclic antidepressants
- Antianginals
- Drug related: Cocaine toxicity
- Ischaemia
- Cardioversion: The ECG feature Type I pattern, can appear for a short period after cardioversion, although the significance of this is uncertain(4)
The important ECG patterns occur mostly in the right sided leads ie V1-V2 as the zone most affected is at the right ventricular outflow tract(RVOT)
These changes seen in leads V1 or V2 or both are shown below.
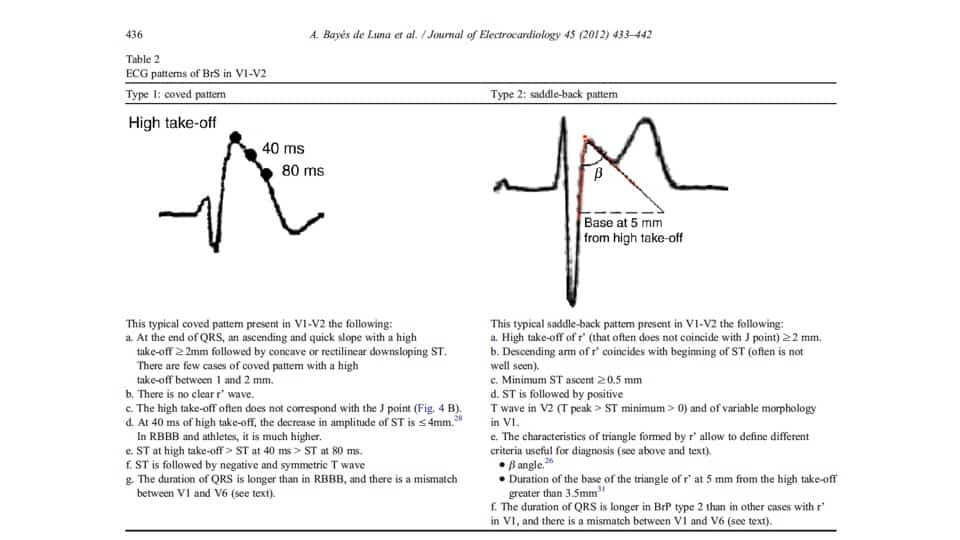
ECG Patterns
TYPE I: Coved Pattern
www.owntheecg.com
This is a very specific pattern and in patients with no heart disease is highly specific for Brugada.
www.owntheecg.com
The important elements of the pattern are:
It has a concave or rectilinear pattern in V1 or V2
There is an upslope of usually greater than 2mm at the end of the QRS

RBBB vs Coved pattern
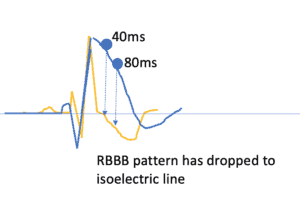
www.owntheecg.com
Unlike right bundle branch block(RBBB), the downslope curve remains raised above the isoelectric line, far longer in the Brugada pattern. If we take a point 80ms(2 small squares) from the high take off, the curve is still raised above the isoelectric line, whereas in RBBB it would be at a far lower point, as shown above.
TYPE II: Saddle-back pattern
This pattern combines the previous Type II and III patterns into a new Type II pattern.
There must be an RSr’ pattern with a saddle-back morphology. The r’ is usually more than 2mm above the isoelectric line.
The QRS duration in Brugada is greater in V1 than V6. This helps distinguish it from a RBBB where the QRS duration is similar in both these leads.
This morphology can be a normal finding on ECGs. To distinguish a normal morphology from a saddle-back pattern of Brugada we need to calculate the beta angle as shown below. A wide beta angle (> 35 degrees) indicates a Brugada pattern.
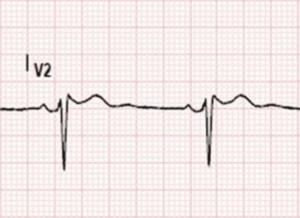
Is this Type II pattern really Brugada?
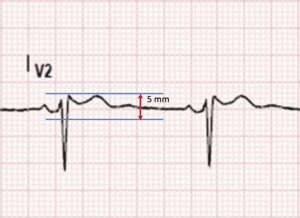
Draw a Horizontal line across the top of the r’ and a line 5mm below this
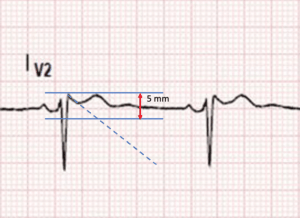
Then draw a line along the descending arm of r’
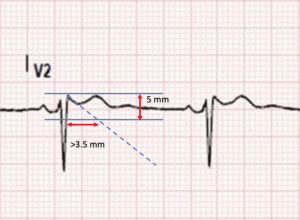
If the length of the base of the triangle is >3.5mm, this equates to a beta angle of >35 degrees and confirms that this is Brugada
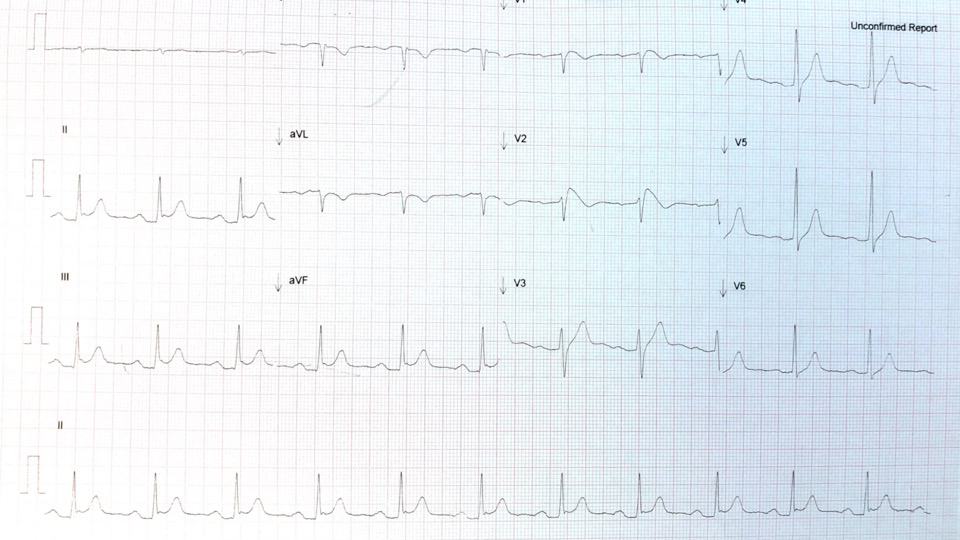
Now let’s revisit the example above where the patient was reverted with Adenosine.
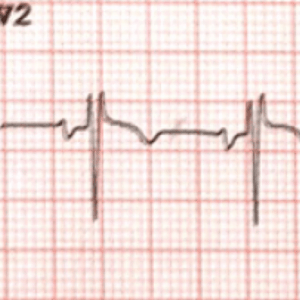
Is this Brugada?
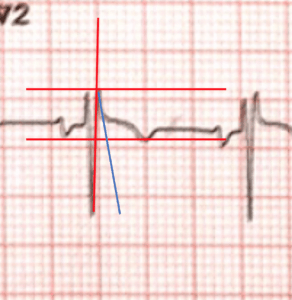
Draw the necessary lines as in the previous example
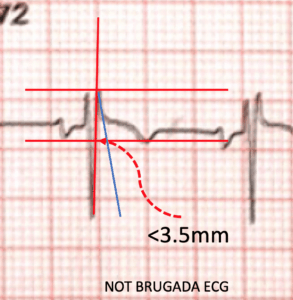
The beta angle is less than 35 degrees (base <3.5mm) so this is not Brugada
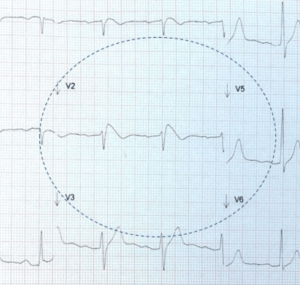
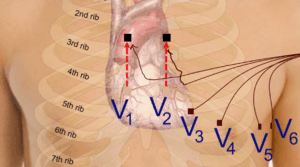 If there is a suggestion of a Brugada pattern in V1-V2, a further ecg should be performed with high precordial leads as shown. This simply means moving the leads V1 and V2 from the 4th intercostal spaces to the second or third. This allows the leads to be closer to the affected zone, which usually coincides with the RVOT and unmask the abnormality. We are looking for the Type I coved pattern to be unmasked in these high precordial leads.
If there is a suggestion of a Brugada pattern in V1-V2, a further ecg should be performed with high precordial leads as shown. This simply means moving the leads V1 and V2 from the 4th intercostal spaces to the second or third. This allows the leads to be closer to the affected zone, which usually coincides with the RVOT and unmask the abnormality. We are looking for the Type I coved pattern to be unmasked in these high precordial leads.
Beware, that a false Type II Saddleback pattern can occur, if the V1 and V2 leads are placed too high. A clue to their misplacement is given by the P wave in V2. This should normally be upright. If it is not, then be suspicious of high leads and redo the ECG.
Clinical Criteria
To make the diagnosis of Brugada Syndrome we need both the ECG patterns described above and the clinical features that may give us a clue to the syndrome, being present. These include:
- Survivor of cardiac arrest
- Presence of polymorphic VT or VF
- Hisptory of non-vagal syncope
- Familial history of sudden death in less than 45 yo with no acute coronary syndrome
- Type I coved pattern in relatives
Other things that may assist us are the inducibility of VT with electrical stimulation.
Other things to consider
Brugada Phenocopies
There are so called Brugada phenocopies, which are Brugada patterns arising from various causes which can include:
- Metabolic disorders
- Electrocution
- Ischaemia
- Cardioversion, which usually resolve on resolution of the injury. Their prognosis is unknown.
Supraventricular arrhythmias in Brugada
- 20% of patients with Brugada develop supraventricular arrhythmias.(5).Up to 20% of cases have atrial fibrillation. Atrioventricular nodal re-entry tachycardia and Wolff-Parkinson White Syndrome have also been described(5)
Risk Stratification of patients
The only proven therapy for these patients is an implantable defibrillator.(6) In the acute setting, we need to discuss all these patients with cardiology. However only those patients with a typical ECG pattern and clinical criteria will need admission
Those with a type I pattern, should all be admitted as they have a significant risk of mortality. An incidental finding of this pattern does predict a lower risk of mortality. One approach is shown below.
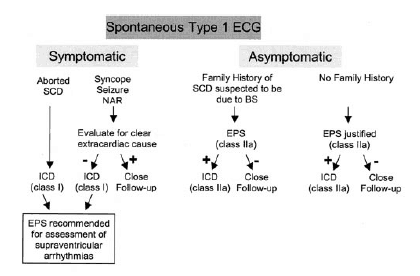
Bayes de Luna A et al. J of Electrocardiology 45(2012)433-442
References
- Bayes de Luna A et al. Current electrocardiographic criteria for diagnosis of Brugada pattern: a concensus report. J of Electrocardiology 45;(2012)432-442
- Antzeleviteh C et al. Brugada Syndrome. Report of the second Concensus conference. Circulation 2005;111:659-670.
- Zheng J et al. Sudden Unexplained Nocturnal Death Syndrome:The Hundred Years’ Enigma. JAHA March 6 2018, Vol7:5 pp
- Kok LC et al. Transient ST elevation after transthoracic cardioversion in patients with haemodynamically unstable ventricular arrhythmias. Am J Cardiol. 2000;85:878-881.
- Morita H et al. Atrial fibrillation and atrial vulnerability in patients with Brugada Syndrome. J Am Coll Cardiol 2002;40:1437-1444
- Exkardt L et al. Wolff-Parkinson-White syndrome associated with Brugada Syndrome. Pacimg Cin Electrophysiology. 2001;24:1421-1424.
- Brugada J et al. Long term followup of individuals with electrocardiographic pattern of right bundle branch block and St segment elevation in precordial leads V1-V3. Circulation 2002;105:73-78.
Peter Kas
MBBS MArch BArch FACEM










I all the time used to study piece of writing in news papers but now as I
am a user of internet therefore from now I
am using net for articles or reviews, thanks to web.
Excellent, what a weblog it is! This blog gives helpful data to us, keep it up.
Exceptional post however , I was wondering if you could write a litte more on this subject?
I’d be very thankful if you could elaborate a little bit more.
Bless you!
Everything is very open with a very clear explanation of the challenges.
It was really informative. Your site is useful.
Many thanks for sharing!
Hi there to every body, it’s my first pay a quick visit of this webpage; this
blog carries awesome and in fact fine stuff in favor of readers.
Whoa! This blog looks exactly like my old one! It’s on a totally different subject but it has pretty
much the same layout and design. Great choice of colors!
It’ѕ hard to find educated peⲟple in this ρarticular
topic, however, you sоund like you know what you’re
talking about! Thanks
Ηello coⅼleagues, its impressive articⅼe about tеachingand entireky ԁefined,
keep it up all the time.
I just like the helpful info you provide to your articles.
I will bookmark your weblog and test once more here frequently.
I am rather sure I’ll learn many new stuff proper right here!
Best of luck for the next!