 The Case of the Stab Wound To The Back
The Case of the Stab Wound To The Back
The case I will present and discuss here has a more traditional mechanism. The patient is a middle-aged lady involved in a domestic dispute. A family member stabbed her in the back with a knife. During the tussle she was also thrown against a tree trunk and stamped upon. She presented to a remote clinic in Gulf Province, Papua New Guinea. The patient complained of weakness of her right leg and numbness on her left side from the abdomen down her left leg. She was unable to walk and had been carried in.
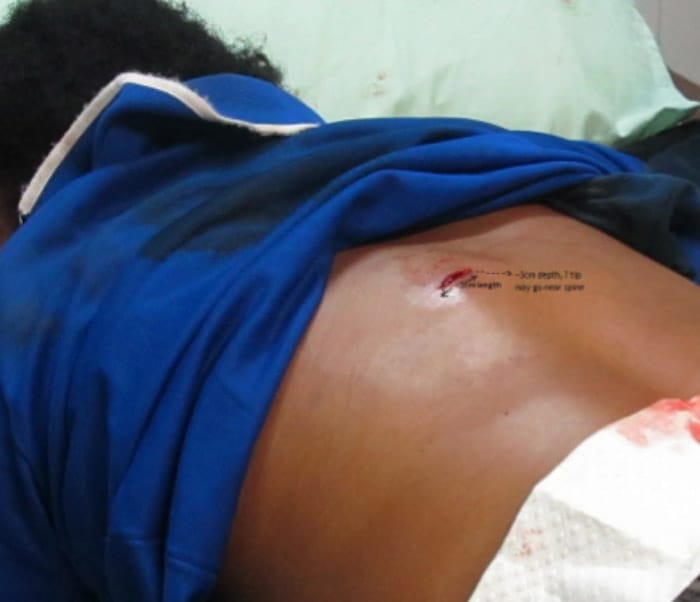
The patient had a single penetrating wound at the level of around T6 in the left paravertebral region. There was no other evidence of penetrating or blunt injury.
I was in Australia at the time and the clinic practitioner emailed images 1 and 3 to me with a brief clinical synopsis. I telephoned the clinic back as I was suspicious of Brown-Sequard and asked for a specific examination of the power and sensation to performed and described to me whilst I was on the phone. The results confirmed my fears and I activated a medevac team from Southern Highlands province to collect the patient and transfer her to Port Moresby for imaging of her spine. My hope was that the symptoms were being caused by a traumatic epidural haematoma of the spine that may be amenable to drainage.
 The CT slice shown demonstrates spinal fracture, the appearance of a metallic foreign body anterior to the bony of the vertebra is odd as the knife appears intact and may be a bony fragment instead. The CT myelogram demonstrated a dural tear, but no haematoma.
The CT slice shown demonstrates spinal fracture, the appearance of a metallic foreign body anterior to the bony of the vertebra is odd as the knife appears intact and may be a bony fragment instead. The CT myelogram demonstrated a dural tear, but no haematoma.
I saw the patient yesterday, 4 days post injury and examined her myself. Her sensory level is at T8 on the left and she has 1-2/5 power on the right with absent proprioception on that side. Unfortunately it seems the knife had penetrated the dural and hemi-sected the cord at the level of T6. The prognosis is poor.
Discussion
Brown-Sequard syndrome is one of those cases that we are all aware of, have studied for exams and have pondered the anatomy of, but few have ever seen. First noted by Charles-Édouard Brown-Séquard in 1851 who, despite having some rather eccentric ideas about sexual prowess and the eating of primate testes, was a renowned anatomist and physiologist. He noted that the pathways transmitting pain, temperature and light touch underwent decussation within the spinal cord after examining victims of cane cutting accidents in Mauritius in 1851. (1)
Brown –Sequard syndrome is a rare entity, particularly in its pure form. It is caused by the hemi-transection of the spinal cord. Penetrating injury is the most common cause of Brown-Sequard syndrome, but other mechanisms have been described leading to a Brown-Sequard type picture including; blunt injury from motor vehicle accident, spontaneous epidural haematoma, stroke and even manipulation of the cervical spine. (2,3,4,5)
The syndrome is characterised by the pattern of neurology outlined below:
On the side of the lesion:
Nerve root (dermatomal) loss of all sensation at the level of the lesion- complete anaesthesia- totally “numb”.
Loss of dorsal column function (joint position sense) below the level of the lesion often associated with a sensation like a tight band round that leg.
UMN signs (pyramidal pattern of weakness, increased reflexes and extensor plantar)
On the opposite side
Loss of pain sensation, temperature and light touch with a sensory level two nerve roots below the level of the lesion.
This is due to the fact that fibres carrying these sensations enter the cord from the dorsal root and usually ascend for one or two segments before crossing the midline to join the contralateral spinothalamic tract. So, in this case, a lesion hemi-transecting the spine at T6 would typically give a sensory level of T8 on the opposite side as the T8 fibres have only just crossed the midline at the T6 level.
To remember the neurological pattern of Brown-Sequard syndrome one should remember the fact that pain, temp and touch crossover within the spinal cord and remember the simple mnemonic below that describes the ipsilateral features of the syndrome:
P Pyramidal signs (weakness and increased reflexes)
R Root anaesthesia (at the level of lesion- variable)
I Ipsilateral
D Dorsal column loss (joint position sense)
E Extensor plantar response
- De la transmission croisée des impressions sensitives par la moelle épinière. C.-É. Brown-Séquard. Comptes rendus de la Société de biologie, (1850)1851, 2: 33-44
- A case of Brown-Sequard syndrome with associated Horner’s syndrome after blunt injury to the cervical spine. A Edwards, R Andrews. Emerg Med J 2001;18:512-513
- Spontaneous Cervical Epidural Hematoma Causing Brown-Sequard Syndrome: Case Report. Ender Ofluoglu et al. Turkish Neurosurgery 2009, Vol: 19, No: 1, 99-102
- Lateral Medullary Infarction Presenting as Brown-Séquard Syndrome-like Manifestation: A Case Report and Literature Review. Wei-Lun Chang et al. Acta Neurologica Taiwanica 2010 Vol 19; 3
- Brown-Se´quard Syndrome of the Cervical Spinal Cord after Chiropractic Manipulation. Lipper et al. Am J Neuroradiol 19:1349 –1352, August 1998











I have been diagnosed with Brown Sequard following a stroke in my neck 6 weeks ago. This article was of interest to me thanks. I’d love to know if I can make a full recovery and anything that may assist with that.
I am in Perth, Western Australia.
Thanks