She is found to be tachycardic, however has no symptoms of palpitations or chest pain or shortness of breath. The ankle injury is not causing significant pain at rest, but the tachycardia continues. She is managed for her ankle injury and discharged.
This same patient had been in the emergency department the day before for initial treatment and was also tachycardic at that time.
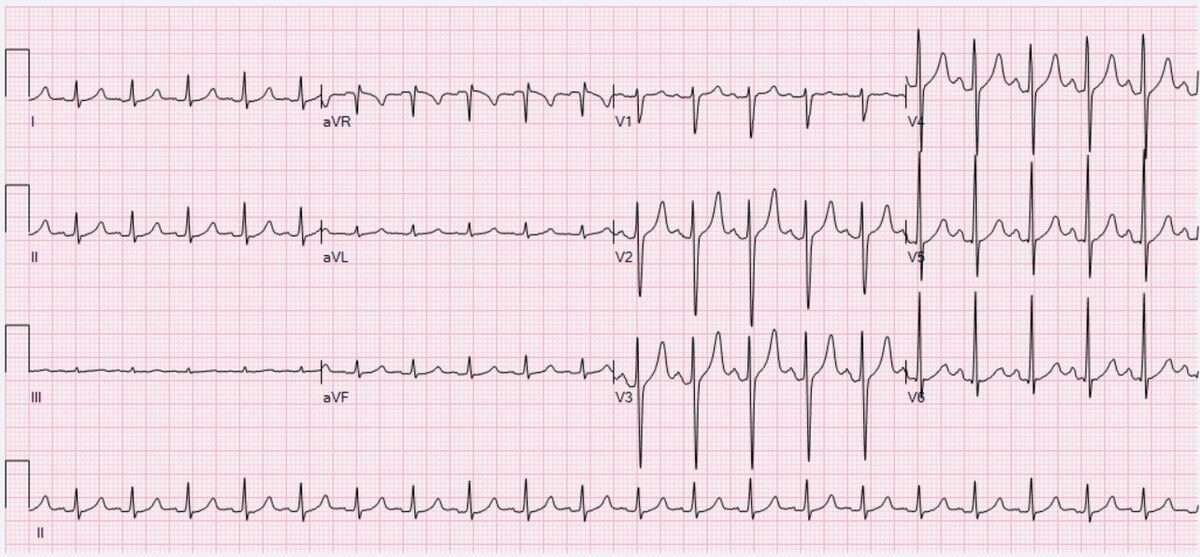
Her ECG is shown below (similar to the patient’s ECG).
What do you think?
This is a straightforward sinus tachycardia.
Why would I have called the patient back when I saw the history?
Persistent sinus tachycardia is worrying.
Simple sinus tachycardia may be caused by responses to pain, drinking coffee or even eating some chocolate, We need to separate the benign from the pathological causes of sinus tachycardia.
These include:
Cardiac:
- Supraventricular tachycardia
- Myocarditis
- Cardiac Tamponade
- Acute coronary syndrome
Non-Cardiac
- Dehydration or Shock
- Respiratory: PE Hypoxia
- Electrolyte Disturbances: hyperkalaemia, hypocalcaemia, hypomagnesaemia
- Haematological: Anaemia, haemolysis
- Endocrine causes: Hyperthyroid, Paheochromocytoma
- Pregnancy
There are many causes of sinus tachycardia. Inappropriate sinus tachycardia is usually associated with symptoms such as palpitations, dyspnoea and dizziness. No cause is found. Trying to control the heart rate in these patients doesn’t always control the symptoms and the usual approach involves decreasing stimulants taking up exercise and controlling fluid and salt intake.
In our patient’s case of an asymptomatic tachycardia at rest and on the background history of diabetes, cardiac autonomic neuropathy is the most probable diagnosis.
What are the subclinical and Clinical Manifestations of cardiac autonomic neuropathy
How do we diagnose it?
What do we have to be on the lookout for?